Biomaterial could keep tooth alive after root canal

A root canal ranks high on most people's list of dreaded dental procedures. Although the lengthy and sometimes painful surgery relieves the agony of an infection, a root canal results in a dead tooth with no living soft tissue, or dental pulp, inside. Today, scientists report development of a peptide hydrogel designed to stimulate the growth of new blood vessels and dental pulp within a tooth after the procedure.
The researchers are presenting their results today at the 256th National Meeting & Exposition of the American Chemical Society (ACS).
"What you end up with after a root canal is a dead tooth," Vivek Kumar, Ph.D., the project's principal investigator, says. "It's no longer responsive. There are no nerve endings or vascular supply. So the tooth is very susceptible to subsequent infection and, ultimately, falling out."
During a root canal, the dentist drills off the top of an infected tooth to access the soft tissue inside. The dentist then removes the infected dental pulp and fills the space with tiny rubber rods called gutta percha and caps the repaired tooth with a crown.
Kumar and Peter Nguyen, Ph.D., who is presenting the work at the meeting, wanted to develop a material that could be injected in place of the gutta percha. The material would stimulate both angiogenesis, or new blood vessel growth, and dentinogenesis, or proliferation of dental pulp stem cells, within the tooth. Both Kumar and Nguyen are at the New Jersey Institute of Technology.
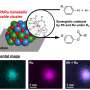
Kumar drew on his previous experience developing a hydrogel that stimulates angiogenesis when injected under the skin of rats and mice. The hydrogel, which is liquid during injection, contains peptides that self-assemble into a gel at the injection site. The peptides contain a snippet of a protein called vascular endothelial growth factor, which stimulates the growth of new blood vessels. Kumar, then a postdoctoral researcher at Rice University, and his coworkers showed that the self-assembling peptide hydrogel stimulated angiogenesis and persisted under the rodents' skin for as long as three months.
"We asked the question, if we can stimulate angiogenesis in a limb, can we stimulate angiogenesis in other regions that have low blood flow?" Kumar says. "One of the regions we were really interested in was an organ in and of itself, the tooth." So Kumar and Nguyen added another domain to the self-assembling angiogenic peptide: a piece of a protein that makes dental pulp stem cells proliferate.
When the team added the new peptide to cultured dental pulp stem cells, they found that the peptide not only caused the cells to proliferate, but also activated them to deposit calcium phosphate crystals—the mineral that makes up tooth enamel. However, when injected under the skin of rats, the peptide degraded within one to three weeks. "This was shorter than we expected, so we went back and redesigned the peptide backbone so that we currently have a much more stable version," says Kumar.
Now, the team is injecting the peptide hydrogel into the teeth of dogs that have undergone root canals to see if it can stimulate dental pulp regeneration in a living animal. If these studies go well, the researchers plan to move the hydrogel into human clinical studies. They have filed a patent for the redesigned peptide.
The hydrogel in its current form likely won't reduce the invasiveness or pain of a root canal, but Kumar and Nguyen are planning future versions of the peptide that contain antimicrobial domains. "Instead of having to rip out everything inside the tooth, the dentist could go in with a smaller drill bit, remove a little bit of the pulp and inject our hydrogel," Kumar says. The antimicrobial portion of the peptide would kill the infection, preserving more of the existing dental pulp, while helping grow new tissue. And the root canal may no longer be such a dreaded procedure.
More information: Dentinogenic self-assembling peptide hydrogels for pulpal tissue regeneration, the 256th National Meeting & Exposition of the American Chemical Society (ACS).
Abstract
Millions of Americans undergo root-canal therapy to treat pulpal degenerative diseases. While the current standard-of-care elastomeric materials, such as gutta percha, are successful in replacing the dental pulp and limiting inflammation in the tissues, they are not intended for tissue regeneration. Self-assembling peptide hydrogels (SAPHs) are versatile platforms that can be modified with functional epitopes to enable diverse biological outcomes. We report a SAPH system modified with dentinogenic functionality enabling the support, proliferation, and targeted differentiation of dental pulp stem cells. These hydrogels are injectable and capable of re-assembling post-injection in situ as demonstrated by oscillatory rheometry and in vivo subcutaneous injection, respectively. We characterized the self-assembly of the hydrogel by electron microscopy and atomic force microscopy and elucidated the secondary structure of the peptide through spectroscopy. In vitro experiments provide evidence for the cytocompatibility of the injectable hydrogel. We demonstrate the efficacy of the hydrogel therapy in animal models and propose the development of the approach for a regenerative alternative to root-canal therapy.
Provided by American Chemical Society