Finding a lethal parasite's vulnerabilities
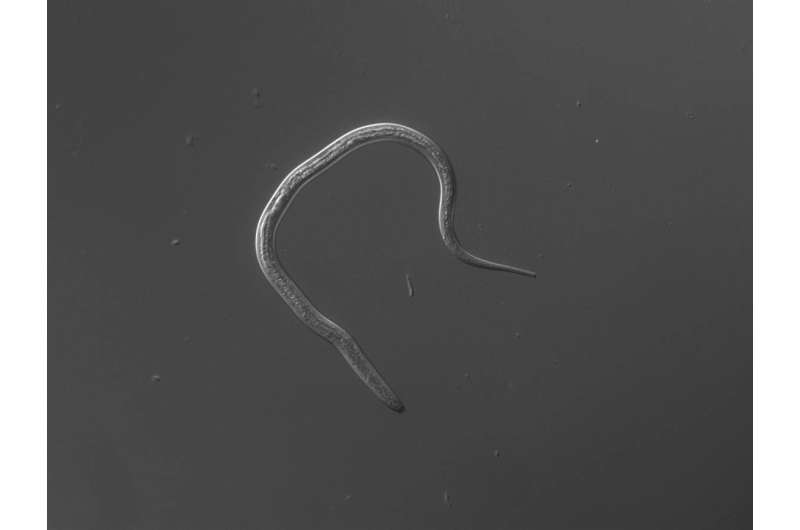
An estimated 100 million people around the world are infected with Strongyloides stercoralis, a parasitic nematode, yet it's likely that many don't know it. The infection can persist for years, usually only causing mild symptoms. But if the immune system is compromised by the use of immunosuppressing drugs such as steroids or chemotherapeutics, for example, the parasite can reproduce uncontrollably, leading to a potentially life-threatening infection.
Researchers from Penn's School of Veterinary Medicine led by James Lok have teamed with labs at Thomas Jefferson University and the University of Texas Southwestern Medical Center to identify the vulnerabilities of this parasite. In a study published last week in the journal Proceedings of the National Academy of Sciences, they showed that, by using a molecule produced naturally by parasites, they could suppress the lethal form of infection in a mouse model of the disease.
"We have the first evidence that this pathway is druggable," says Lok, a professor of parasitology at Penn Vet and a co-corresponding author on the study. "We have a lot of work yet to do, but the fact that we have a small, relatively stable molecule that can intervene in an infection like this is very encouraging."
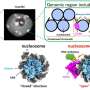
Humans acquire Strongyloides when the skin comes into contact with contaminated soil. Unlike other nematode parasites, Strongyloides has the unique ability to carry out its entire life cycle within a human host, a state known as autoinfection. After third-stage larvae (L3i) penetrate the skin and travel to the gut, some can develop into autoinfective third-stage larvae (L3a), triggering a persistent cycle of infection in the host. A treatment exists for Strongyloides, but it is not always available and there is evidence that related parasites are beginning to develop resistance against it.
The researchers wanted to see if they could prevent the formation of these L3a larvae as a way of stemming the parasite's ability to reproduce inside the host's body. While mice are normally resistant to Strongyloides infection, the team identified an immunocompromised mouse model that was susceptible, and that developed a lethal form of infection, known as "hyperinfection," after treatment with a steroid.
In earlier work, researchers on the team had found that a chemical produced by other nematodes, Δ7-dafachronic acid, regulates many aspects of the worms' development, including the ability of L3i to transform into L3a. To see if this chemical might reduce formation of L3a inside of an infected host, the team gave the infected mice two different doses of the chemical, and found it reduced the parasite burden in a dose-dependent manner.
"That dose response was an essential quality for assigning causality to this treatment," Lok says. "Where we had a suggestive downward trend at 1 micromolar Δ7-dafachronic acid, at 10 micromolar we had a significant trend toward fewer of the third-stage autoinfective larvae."
In future work, the labs hope to continue collaborating to see whether such an approach might work to treat other parasitic worms, such as hookworm, which affects half a billion people around the world each year. It could also prove effective against related parasites that harm livestock and agricultural crops, Lok notes.
Additionally, the scientists hope to build off of the success in using the naturally occurring Δ7-dafachronic acid to synthesize a compound that might lend itself better to therapeutic treatment.
"The worms have given us a lead," Lok says. "Now we need to work on this from a medicinal chemical standpoint to find a drug that can persist in the host, have minimal side effects, and be orally available—all things you want to see in a therapy that is going to be used in many under-resourced areas around the globe."
More information: John B. Patton et al, Methylprednisolone acetate induces, and Δ7-dafachronic acid suppresses,Strongyloides stercoralishyperinfection in NSG mice, Proceedings of the National Academy of Sciences (2017). DOI: 10.1073/pnas.1712235114
Journal information: Proceedings of the National Academy of Sciences
Provided by University of Pennsylvania