Staphylococcus aureus has a resistance strategy that thwarts certain antimicrobials
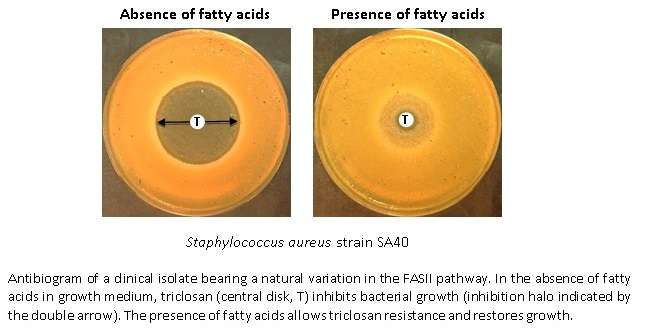
The natural presence of fatty acids in the human body leads to increased resistance of Staphylococcus aureus to a class of antimicrobials that target bacterial fatty acid biosynthesis. This discovery, based on research by INRA scientists in collaboration with with INSERM, Hôpital Cochin APHP, the Université Paris Descartes, Institut Pasteur and CNRS scientists, is reported in an article in Nature Communications (5 October 2016). While antimicrobial drug discovery is a top research priority, this work reveals that resistance strategies involving host fatty acids can thwart the use of fatty acid synthesis inhibitors to treat staphylococcal infection.
Triclosan is an antibacterial agent widely used in household products (mouthwash, toothpaste, lotion, shower gel), and in health care (sanitizers, surgical sutures). It belongs to a family of antimicrobials that inhibit synthesis of fatty acids (called FASII, for type II fatty acid synthesis), which are vital bacterial components. Triclosan was recently removed by the European Commission from its list of approved additives in Type 1 products (household products) due to potential health risks and questionable benefits. The American Food and Drug Administration (FDA) also banned its use in antibacterial soaps in 2016. However, triclosan remains in use, and new FASII inhibitors are in development for future use as antibiotics.
In 2009, a study conducted by teams from INRA, Inserm, Hôpital Cochin APHP, the Université Paris Descartes, Institut Pasteur and the CNRS showed that Gram-positive bacteria (streptococcus, enterococcus, and staphylococcus) can develop in the presence of FASII inhibitors by using the fatty acids found in human blood. However, the capacity of the major human pathogen Staphylococcus aureus to overcome FASII inhibitors remained in debate.
The same teams then focused on Staphylococcus aureus growth in environments containing fatty acids in combination with triclosan. They demonstrated that fatty acids promote about 100-fold increases in mutations that confer triclosan resistance. Some of these resistant bacteria synthesized their own fatty acids in a normal way when triclosan was not present, but then could overcome this FASII inhibitor by efficiently incorporating the environmental fatty acids. A strain with these properties was fully virulent, indicating that the biological cost of the mutation responsible for resistance is low. In fact, database searches of staphylococcal genomes revealed that this mutation is already present in some clinical isolates; as expected, these strains proved to be triclosan resistant.
Human skin and nares, which are rich in fatty acids, are naturally colonized by bacteria including staphylococci. These could be privileged locations for developing resistant bacteria when using topical products containing FASII inhibitors like triclosan. This research indicates that treating staphylococcal infections with FASII inhibitors, or using consumer products containing them, may favor the emergence or spread of resistant staphylococci. It highlights the importance of studying bacterial responses to antimicrobials in growth conditions mimicking natural colonization or infection environments – i.e., with human fatty acids – when developing new anti-FASII antibiotics.
More information: Claire Morvan et al. Environmental fatty acids enable emergence of infectious Staphylococcus aureus resistant to FASII-targeted antimicrobials, Nature Communications (2016). DOI: 10.1038/NCOMMS12944
Journal information: Nature Communications
Provided by INRA-France