Genomes of chimpanzee parasite species reveal evolution of human malaria

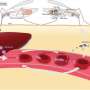
Understanding the origins of emerging diseases - as well as more established disease agents—is critical to gauge future human infection risks and find new treatment and prevention approaches. This holds true for malaria, which kills more than 500,000 people a year. Symptoms, including severe anemia, pregnancy-associated malaria, and cerebral malaria, have been linked to the parasite's ability to cause infected red blood cells to bind to the inner lining of blood vessels.
An international team led by Beatrice Hahn, MD, a professor of Medicine and Microbiology from the Perelman School of Medicine at the University of Pennsylvania, and MD/PhD student Sesh Sundararaman, used a selective amplification technique to sequence the genomes of two divergent Plasmodium species, Plasmodium reichenowi and Plasmodium gaboni, from miniscule volumes of chimpanzee blood to find clues about the evolution and pathogenicity of Plasmodium falciparum, the deadliest malaria parasite that affects people. Their findings appear this week in Nature Communications.
African apes harbor at least six Plasmodium species that have been classified into a separate subgenus, called Laverania. Three of these Laverania species, including Plasmodium reichenowi and Plasmodium gaboni, reside in chimps, while three others, including Plasmodium praefalciparum that gave rise to Plasmodium falciparum, reside in gorillas. The gorilla origin of Plasmodium falciparum was discovered several years ago by this same international group of investigators.
"We want to know why Plasmodium falciparum is so deadly," Hahn said. "The answer must lie in the blueprint—the genome—of its chimpanzee and gorilla cousins. We also want to know how and when the gorilla precursor of Plasmodium falciparum jumped into humans, and why this happened only once."
Parasites infecting humans and great apes share genes that allow them to hide from the host's immune system, adhere to tissues, and cause disease. Better understanding the evolution of human malaria virulence provides potential new targets for drugs and vaccines.
Coauthor Dustin Brisson, PhD, a professor of Biology at Penn, initially developed the selective amplification method to sequence bacterial genomes. Sundararaman calls applying this new approach to malaria research "one of the paper's most important contributions." Using this technique, the team was able to generate high quality Laverania genome sequences by using small amounts of unprocessed blood collected from chimpanzees living in sanctuaries during routine health screens.
The chimpanzee parasite genomes contain a goldmine of information about the evolutionary origins of the malaria parasites infecting humans. One of the first things to emerge from genome-wide analyses was that the parasites indeed represent distinct, non-interbreeding species.
In addition, members of each chimpanzee parasite species display about 10 times more genetic diversity than do human parasites. "The chimpanzee parasites really highlight the lack of diversity in Plasmodium falciparum," said co-author Paul Sharp, PhD, an evolutionary biologist from the University of Edinburgh and long-term collaborator of the Hahn team. "This is most likely because these parasites went through a severe bottleneck when first transmitted to humans, perhaps within the past 10,000 years."
By comparing the different parasite genomes the team also found an expansion of a multi-gene family, which governs red blood cell remodeling and therefore helps the parasite to evade host immune cells as well as clearance by the spleen. "The remodeling process is a key part of severe malaria pathology in human Plasmodium falciparum infections," explained coauthor Julian Rayner, PhD, a malaria researcher at the Wellcome Trust Sanger Institute and long-term member of the research team. "The expansion of this gene family from a single gene in all other Plasmodium parasites to up to 21 genes in Laverania suggests that remodeling evolved early in the radiation of this group of primate parasites and contributed not only to their unique biology but perhaps also to their successful expansion."
"'We also found a short region of the genome, including two essential invasion genes, where Plasmodium falciparum was much more different from its close relatives than we expected," said Lindsey Plenderleith, PhD, a postdoctoral fellow at the University of Edinburgh, who together with Sundararaman compared and annotated the various parasite genomes. Further analysis yielded the surprising finding that this fragment of DNA was horizontally transferred—from one species to another—into the gorilla ancestor of Plasmodium falciparum.
"It is tempting to speculate that this unusual event somehow predisposed the precursor of Plasmodium falciparum to colonize humans," added Hahn. "However, this gene transfer clearly is not the entire story."
Although the origin of Plasmodium falciparum is now well-established from past research by this group, nothing is known about the circumstances that led to its emergence. "Coaxing entire parasite genome sequences out of small quantities of unprocessed ape blood will help us to better understand what happened and whether it can happen again," Sundararaman said.
"It's an exciting time to study Plasmodium species that cannot be cultured and have thus been neglected because of the difficulty of obtaining sufficient quantities of DNA for whole genome sequencing," Hahn said. The team plans, as a next step, to use the now validated select genome amplification technique to sequence additional ape parasite genomes to identify host-specific interactions and transmission requirements, thereby uncovering vulnerabilities that can be exploited to combat human malaria.
Colleagues from the Sanaga-Yong Chimpanzee Rescue Center, IDA-Africa, Portland, OR, and the Institut de Recherche pour le Developpement (IRD), Montpellier, France, were also coauthors.
Journal information: Nature Communications
Provided by University of Pennsylvania School of Medicine