Making a better wound dressing—with fish skin
With a low price tag and mild flavor, tilapia has become a staple dinnertime fish for many Americans. Now it could have another use: helping to heal our wounds. In the journal ACS Applied Materials & Interfaces, scientists have shown that a protein found in this fish can promote skin repair in rats without an immune reaction, suggesting possible future use for human patients.
Jiao Sun, Xiumei Mo and colleagues explain that applying collagen—a major structural protein in animals—to wounds can help encourage skin to heal faster. But when the protein dressing comes from mammals such as cows and pigs, it has the potential to transmit conditions such as foot-and-mouth disease. Searching for an alternative source of collagen, scientists recently turned to the ocean. Sun's team wanted to test fish collagen's potential as a more benign wound treatment.
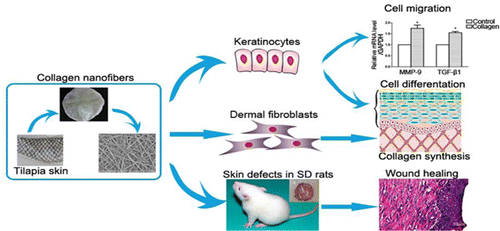
The researchers developed nanofibers from tilapia collagen and used them to cover skin wounds on rats. The rats with the nanofiber dressing healed faster than those without it. In addition, lab tests on cells suggested that the fish collagen was not likely to cause an immune reaction. The researchers conclude that it could be a good candidate to develop for clinical use.
More information: Development of Biomimetic Tilapia Collagen Nanofibers for Skin Regeneration through Inducing Keratinocytes Differentiation and Collagen Synthesis of Dermal Fibroblasts, ACS Appl. Mater. Interfaces, 2015, 7 (5), pp 3253–3262. DOI: 10.1021/am507990m
Abstract
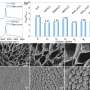
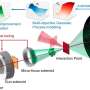
In this study, tilapia skin collagen sponge and electrospun nanofibers were developed for wound dressing. The collagen sponge was composed of at least two α-peptides, and its denaturation temperature was 44.99 °C. It did not change the number of spleen-derived lymphocytes in BALB/c mice, the ratio of CD4+/CD8+ lymphocytes, and the level of IgG or IgM in Sprague–Dawley rat. The contact angle, tensile strength, and weight loss temperature of collagen nanofibers were 21.2°, 6.72 ± 0.44 MPa, and 300 °C, respectively. The nanofibers could promote the viabilities of human keratinocytes (HaCaTs) and human dermal fibroblasts (HDFs), inducing epidermal differentiation through the gene expression of involucrin, filaggrin, and type I transglutaminase of HaCaTs, and they could also accelerate migration of HaCaTs with the expression of matrix metalloproteinase-9 and transforming growth factor-β1 (TGF-β1). Besides, the nanofibers could upregulate the protien level of Col-I in HDFs both via a direct effect and TGF-β1 secreted from HaCaTs, thus facilitating the formation of collagen fibers. Furthermore, the collagen nanofibers stimulated the skin regeneration rapidly and effectively in vivo. These biological effects could be explained as the contributions from the biomimic extracellular cell matrix structure, hydrophilicity, and the multiple amino acids of the collagen nanofibers.
Journal information: ACS Applied Materials and Interfaces
Provided by American Chemical Society