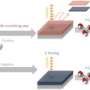
Wireless electronic implants stop staph, then dissolve
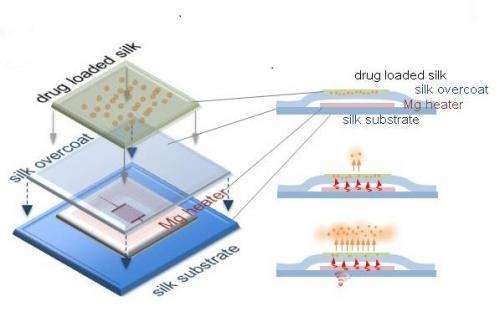
Researchers at Tufts University, in collaboration with a team at the University of Illinois at Champaign-Urbana, have demonstrated a resorbable electronic implant that eliminated bacterial infection in mice by delivering heat to infected tissue when triggered by a remote wireless signal. The silk and magnesium devices then harmlessly dissolved in the test animals. The technique had previously been demonstrated only in vitro. The research is published online in the Proceedings of the National Academy of Sciences Early Edition the week of November 24-28, 2014.
"This is an important demonstration step forward for the development of on-demand medical devices that can be turned on remotely to perform a therapeutic function in a patient and then safely disappear after their use, requiring no retrieval," said senior author Fiorenzo Omenetto, professor of biomedical engineering and Frank C. Doble professor at Tufts School of Engineering. "These wireless strategies could help manage post-surgical infection, for example, or pave the way for eventual 'wi-fi' drug delivery."
Implantable medical devices typically use non-degradable materials that have limited operational lifetimes and must eventually be removed or replaced. The new wireless therapy devices are robust enough to survive mechanical handling during surgery but designed to harmlessly dissolve within minutes or weeks depending on how the silk protein was processed, noted the paper's first author, Hu Tao, Ph.D., a former Tufts post-doctoral associate who is now on the faculty of the Shanghai Institute of Microsystem and Information Technology, Chinese Academy of Sciences.
Each fully dissolvable wireless heating device consisted of a serpentine resistor and a power-receiving coil made of magnesium deposited onto a silk protein layer. The magnesium heater was encapsulated in a silk "pocket" that protected the electronics and controlled its dissolution time.
Devices were implanted in vivo in S. aureus infected tissue and activated by a wireless transmitter for two sets of 10-minute heat treatments. Tissue collected from the mice 24 hours after treatment showed no sign of infection, and surrounding tissues were found to be normal. Devices completely dissolved after 15 days, and magnesium levels at the implant site and surrounding areas were comparable to levels typically found in the body.
The researchers also conducted in vitro experiments in which similar remotely controlled devices released the antibiotic ampicillin to kill E. coli and S. aureus bacteria. The wireless activation of the devices was found to enhance antibiotic release without reducing antibiotic activity.
More information: "Silk-based resorbable electronic devices for remotely controlled therapy and in vivo infection abatement," PNAS, www.pnas.org/cgi/doi/10.1073/pnas.1407743111
Journal information: Proceedings of the National Academy of Sciences
Provided by Tufts University