Human scabs serve as inspiration for new bandage to speed healing

Human scabs have become the model for development of an advanced wound dressing material that shows promise for speeding the healing process, scientists are reporting. Their study appears in the journal ACS Applied Materials & Interfaces.
Shutao Wang and colleagues explain that scabs are a perfect natural dressing material for wounds. In addition to preventing further bleeding, scabs protect against infection and recruit the new cells needed for healing. Existing bandages and other dressings for wounds generally are intended to prevent bleeding and infections. Wang's team set out to develop a new generation of wound dressings that reduce the risk of infections while speeding the healing process.
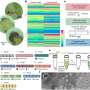
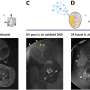
They describe how research on the surface structure of natural scabs served as inspiration for developing a "cytophilic" wound dressing material. It attracts new cells needed for healing. The material mimics the underside of scabs, where tiny fibers are arranged in the same direction like velvet or a cat's fur. Wang's team spun fibers of polyurethane—the common durable and flexible plastic—into the same pattern. In laboratory experiments, the human cells involved in healing quickly attached to the membrane and lined up like those in actual scabs. The scientists conclude that this membrane "is of great potential in fabricating dressing materials for rapid wound healing, as well as other biomaterials, such as membrane for capturing circulating tumor cells, bone growth and constructing neural networks."
The article is titled "Scab-Inspired Cytophilic Membrane of Anisotropic Nanofibers for Rapid Wound Healing."
More information: Scab-Inspired Cytophilic Membrane of Anisotropic Nanofibers for Rapid Wound Healing, ACS Appl. Mater. Interfaces, Article ASAP. DOI: 10.1021/am4004683
Abstract
This work investigates the influence of cytophilic and anisotropic nanomaterials on accelerated cell attachment and directional migration toward rapid wound healing. Inspired by the anisotropic protein nanofibers in scab, a polyurethane (PU) nanofibrous membrane with an aligned structure was fabricated. The membrane showed good affinity for wound-healing-related cells and could guide cell migration in the direction of PU nanofibers. Also, the morphology and distribution of F-actin and paxillin of attached cells were influenced by the underlying nanofibers. The randomly distributed PU nanofibers and planar PU membrane did not show a distinct impact on cell migration. This scab-inspired cytophilic membrane is promising in applications as functional interfacial biomaterials for rapid wound healing, bone repair, and construction of neural networks.
Journal information: ACS Applied Materials and Interfaces
Provided by American Chemical Society