The entwined destinies of mankind and leprosy bacteria
Leprosy still affects hundreds of thousands of people today throughout the entire world. An international team headed by EPFL professor Stewart Cole has traced the history of the disease from ancient Egypt to today and in doing so has made a public health study essential for combating the disease.
For thousands of years an undesirable and persistent companion has been travelling with man wherever he goes. Mycobacterium leprae, the bacterium that causes leprosy, has only one known natural host - mankind. And because of man's many travels, this bacillus has colonized the entire earth. Its history is therefore intimately tied to our own, and it is this migratory relationship that Stewart Cole, EPFL (Switzerland) professor of Microbial Pathogenesis, and his team have analyzed in a study to be published in Nature Genetics. Geneticists, microbiologists, and even archeologists have followed the bacteria's traces from their lab to the Silk Road and the tombs of Egyptian mummies.
The scientists started with the past history of the disease by investigating the remains of English, Croatian, and Bulgarian medieval cemeteries along with an ancient Egyptian burial site to find traces of the bacteria's DNA. "A person infected with the bacteria shows specific signs of bone deformations, like hands gripped closed in the form of a claw," explains Steward Cole, "and these clues helped us determine if we were dealing with the bodies of people who died from the disease."
In the wake of commercial ships
Even though Egypt is geographically close to East Africa, where one of the four strains of leprosy comes from, DNA from a 4th century mommy shows traces of the European strain. Not necessarily surprising, for the Pharaonic Empire was economically and culturally tied to the old continent. With humans being the only possible vessel for the bacteria, it naturally navigated along with man throughout the trade routes of the seas.
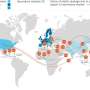
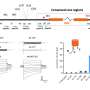
The four strains of the leprosy bacilli that the scientific team found are: European, East African, West African and Indian. Their current distribution around the world echoes the history of population movements. Other examples in the study include Madagascar where, in spite of its geographic proximity to the African coast, the Indian strain is found on the island, where the majority of the inhabitants are of Indian origin. In Brazil, the West African strain is dominant, a probable consequence of the slave trade, but we also find the European strain - brought most likely from colonization.
"One of the most interesting surprises is the discovery that the bacteria found in China are of European origin," explains Stewart Cole, "and one would have naturally expected the Indian strain. The most probable explanation is that the strain was carried by traders along the Silk Road."
A stable DNA, more efficient treatments
There is little doubt that the bacillus originated in East Africa - Stewart Cole will examine this hypothesis in a future study - and then mutated into the four different strains. "The results of our analysis are surprising," says Cole, "the difference between the different strains is very small. It is one of the most stable organisms ever observed, even if half of its genome is dead." There are only around a hundred different variations between the DNA of two different strains, whereas with HIV or the flu there may be thousands of difference mutations.
In the case of HIV, mutations are so frequent that it is almost possible to say whether a person was infected in Geneva or in Lausanne," explains Stewart Cole, "but in the case of leprosy, the most we can do is place the infection on a continental scale." But this is not bad news. Frequent mutation by a bacterium often leads to disturbing resistances to antibiotic treatments, such as with tuberculoses. But a more stable bacillus responds more efficiently to treatment regardless of the strain. "Resistant cases are extremely rare for leprosy."
Yet the disease remains a persistent public health issue in certain regions in India and Brazil. Currently, more than 700,000 people are infected world-wide and the length of treatment of at least one year can complicate its application. We have not yet head the last from Mycobacterium leprae, but public health politics, spurred on by work done by the likes of Stewart Cole and his scientific team, could put an end to the common history between leprosy and its unwilling human host.
More information: The scientific article in Nature Genetics: www.nature.com/ng/journal/vaop … ent/full/ng.477.html
Source: Ecole Polytechnique Fédérale de Lausanne