Researchers find reproductive germ cells survive and thrive in transplants, even among species
Reproductive researchers from the University of Pennsylvania and The Children's Hospital of Philadelphia have succeeded in isolating and transplanting pure populations of the immature cells that enable male reproduction in two species—human spermatogonia and mouse gonocytes. These germline stem cells, taken from testis biopsies, demonstrated viability following transplantation to mouse testes within a controlled laboratory setting.
The results indicate remarkable similarity between the gene expression and behavior of the ancient cells that govern reproduction, even between two species that diverged phylogenetically 75 million years ago. The study reveals much about the lifecycle of the male germline stem cell. The results demonstrate relevance to the basic understanding of all stem cell types—which are frequently difficult to isolate in such highly enriched populations—but also provide hope to prepubescent men risking infertility due to cancer treatment. A clinical trial using this methodology is underway at CHOP.
"There is remarkable similarity between prepubertal human spermatogonia and mouse gonocytes, which is not only very surprising but quite informative considering the large separation between human and mouse," said Ralph L. Brinster, a reproductive physiologist at the University of Pennsylvania School of Veterinary Medicine. "In our studies we found seven of the 100 most highly enriched genes between germ cells and somatic cells were conserved in human and mice, attesting to the fundamental importance of germ cells in species evolution."
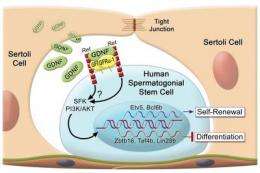
Even when human prepubescent germ cells were transplanted into mouse testes, the cells preserved themselves by migrating to the "basement" membrane of the seminiferous tubule where they were maintained for months. The expression of several novel genes known to be essential for stem cell self-renewal was high.
The ability of prepubertal human spermatogonia to migrate to the basement membrane of mouse testes and be maintained as germ cells, and likely spermatogonial stem cells (SSCs), lends biological support to the similarity of the two species' germ cells. The relationship opens a window of opportunity to learn about human SSCs through studies on prepubertal human spermatogonia that can be identified and isolated in essentially pure populations and relating observations to the rapidly developing information base about mouse SSCs.
The research team, led by Brinster and Jill P. Ginsberg, pediatric oncologist with The Children's Hospital of Philadelphia, published the study, "Prepubertal Human Spermatogonia and Mouse Gonocytes Share Conserved Gene Expression of Germline Stem Cell Regulatory Molecules," Dec. 14, 2009 in the journal Proceedings of the National Academy of Sciences.
The results have particular relevance to medical treatment of human infertility because of the critical role of these stem cells in male fertility. With cure rates of childhood cancer now approaching 80, about one in 640 individuals of reproductive age are now cancer survivors. However, many of these survivors will have fertility problems as adults. Cryopreservation of a testis biopsy in a tissue bank from boys undergoing cancer therapy is an option to preserve stem cells for later transplantation to restore spermatogenesis and is currently being examined in clinical trials. The results in the paper provide valuable information relevant to handling stem cells during cryopreservation and transplantation and also establish a foundation for culture studies on the stem cells.
The Children's Hospital of Philadelphia is currently offering testicular tissue cryopreservation as an experimental treatment option. The study began in January 2008 and includes 16 boys diagnosed with various solid tumors, ranging in age from 3 months to 14 years old. All were treated with chemotherapy or radiation, which carries a significant risk of resulting infertility. These boys had a tiny portion of their testis removed and frozen for their potential future use. The hope is one day to use frozen tissue from prepubescent males to restore fertility. Physicians would thaw the preserved tissue and reimplant it in the patient's testes, or use it for other assisted reproduction technologies.
"Even though there are currently no guarantees of clinical success, families are highly receptive to this option," said Ginsberg, who led the clinical arm of the research study. Results of that study, demonstrating whether parents would be receptive to the treatment option, were published online Oct. 27 in the journal Human Reproduction.
Provided by University of Pennsylvania














