Stem cells replace stroke-damaged tissue in rats
Effective stem cell treatment for strokes has taken a significant step forward today as scientists reveal how they have replaced stroke-damaged brain tissue in rats.
The team of scientists is funded by the Biotechnology and Biological Sciences Research Council (BBSRC) and led by Dr Mike Modo of the Institute of Psychiatry, King's College London. The work, carried out at the Institute of Psychiatry and University of Nottingham, shows that by inserting tiny scaffolding with stem cells attached, it is possible to fill a hole left by stroke damage with brand new brain tissue within 7 days. The work is published in Biomaterials.
Previous experiments where stem cells have been injected into the void left by stroke damage have had some success in improving outcomes in rats. The problem is that in the damaged area there is no structural support for the stem cells and so they tend to migrate into the surrounding healthy tissues rather than filling up the hole left by the stroke.
Dr Modo said: "We would expect to see a much better improvement in the outcome after a stroke if we can fully replace the lost brain tissue, and that is what we have been able to do with our technique."
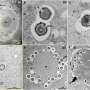
Using individual particles of a biodegradable polymer called PLGA that have been loaded with neural stem cells, the team of scientists have filled stroke cavities with stem cells on a ready-made support structure.
Dr Modo continued: "This works really well because the stem cell-loaded PLGA particles can be injected through a very fine needle and then adopt the precise shape of the cavity. In this process the cells fill the cavity and can make connections with other cells, which helps to establish the tissue.
"Over a few days we can see cells migrating along the scaffold particles and forming a primitive brain tissue that interacts with the host brain. Gradually the particles biodegrade leaving more gaps and conduits for tissue, fibres and blood vessels to move into."
The research published today uses an MRI scanner to pinpoint precisely the right place to inject the scaffold-cell structure. MRI is also used to monitor the development of the new brain tissue over time.
The next stage of the research will be to include a factor called VEGF with the particles. VEGF will encourage blood vessels to enter the new tissue.
Professor Douglas Kell, BBSRC Chief Executive said: "Stroke is a leading cause of disability in industrialised countries. It is reassuring to know that the technology for treating stroke by repairing brain damage is getting ever closer to translation into the clinic. This crucial groundwork by Dr Modo and his colleagues will surely be a solid foundation of basic research for much better treatments in the future."
Joe Korner, Director of Communications at The Stroke Association commented: "This research is another step towards using stem cell therapy in treating and reversing the brain damage caused by stroke. It is exciting because researchers have shown they are able to overcome some of the many challenges in translating the potential of using stem cells into reality.
"The potential to reverse the disabling effects of stroke seems to have been proved. However the development of stem cell therapy for stroke survivors is still in the early stages and much more research will be needed before it can be tested in humans or used in practice.
"Every five minutes someone in the UK has a stroke and it is vital that we do all we can to help those affected by stroke."
Source: Biotechnology and Biological Sciences Research Council