Hormone therapy could enhance the therapeutic effect of head and facial bone grafts
Bone grafts, which are used to treat head injuries and birth defects, still pose major medical challenges, but scientists are reporting progress toward a new hormone therapy that could improve the outcomes of these surgeries. Their study, which was conducted on mice, appears in the ACS journal Molecular Pharmaceutics.
Zulma Gazit at Cedars-Sinai Medical Center, Edward Schwarz from Rochester University and colleagues note that surgeons perform nearly 100,000 head and facial bone-grafting procedures every year to treat bone loss from disease, birth defects or traumatic injuries. Though this kind of reconstructive surgery dates back to ancient times, the options for implant materials remain limited. Doctors can remove bone from another part of a patient's body or use lab-made materials, but these methods can lead to serious complications. Currently, one of the preferred alternatives is to use bone grafts received from tissue banks, but they often don't join with the bone they're supposed to fix. Preliminary studies have shown that parathyroid hormone (PTH), a drug approved by the U.S. Food and Drug Administration to treat osteoporosis, helps repair fractures in long bones. The team wanted to see if PTH also would help head and facial donor grafts fuse into place.
They tested the hormone in mice with skull defects that they implanted with donor grafts. Daily short-term PTH treatment improved bone formation around the grafts and prevented scar tissue, which can interfere with graft integration, from forming. "These findings will aid in the development of an attractive bone graft, which is readily available, for use in craniofacial reconstruction," they say.
More information: "PTH Promotes Allograft Integration in a Calvarial Bone Defect" Mol. Pharmaceutics, Article ASAP. DOI: 10.1021/mp400292p
Abstract
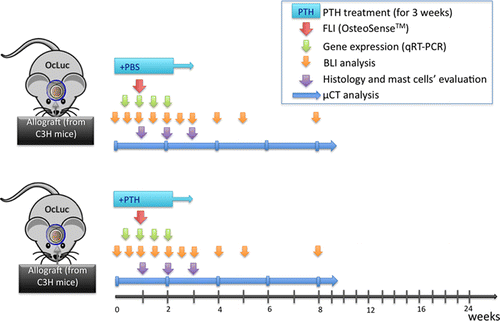
Allografts may be useful in craniofacial bone repair, although they often fail to integrate with the host bone. We hypothesized that intermittent administration of parathyroid hormone (PTH) would enhance mesenchymal stem cell recruitment and differentiation, resulting in allograft osseointegration in cranial membranous bones. Calvarial bone defects were created in transgenic mice, in which luciferase is expressed under the control of the osteocalcin promoter. The mice were given implants of allografts with or without daily PTH treatment. Bioluminescence imaging (BLI) was performed to monitor host osteprogenitor differentiation at the implantation site. Bone formation was evaluated with the aid of fluorescence imaging (FLI) and microcomputed tomography (μCT) as well as histological analyses. Reverse transcription polymerase chain reaction (RT-PCR) was performed to evaluate the expression of key osteogenic and angiogenic genes. Osteoprogenitor differentiation, as detected by BLI, in mice treated with an allograft implant and PTH was over 2-fold higher than those in mice treated with an allograft implant without PTH. FLI also demonstrated that the bone mineralization process in PTH-treated allografts was significantly higher than that in untreated allografts. The μCT scans revealed a significant increase in bone formation in allograft + PTH treated mice comparing to allograft + PBS treated mice. The osteogenic genes osteocalcin (Oc/Bglap) and integrin binding sialoprotein (Ibsp) were upregulated in the allograft + PTH treated animals. In summary, PTH treatment enhances osteoprogenitor differentiation and augments bone formation around structural allografts. The precise mechanism is not clear, but we show that infiltration pattern of mast cells, associated with the formation of fibrotic tissue, in the defect site is significantly affected by the PTH treatment.
Journal information: Molecular Pharmaceutics
Provided by American Chemical Society