Long-term disability claims dominate benefits litigation, study says
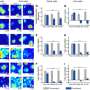
An empirical study of employee benefits litigation from 2006 to 2010 reveals that cases involving long-term disability claims accounted for over 60 percent of all federal cases among five broad categories, including health care, life and accidental death, and pension cases.
Sean M. Anderson, a University of Illinois expert in employee benefit plan policy and regulation, says the prevalence of litigation involving long-term disability plans is particularly striking because fewer private employees participate in disability plans than in other types of plans.
"Even though there are fewer people involved in disability plans, they generate a disproportionate share of the litigation that's happening," said Anderson, a law lecturer whose study was published in the ABA Journal of Labor & Employment Law.
According to the article, Department of Labor statistics released in 2009 showed that only 38 percent of private industry workers participated in short-term disability plans and only 31 percent in long-term disability plans, whereas 52 percent participated in medical benefit plans, 57 percent in life insurance plans and 51 percent in qualified pension plans.
"It's interesting that only 31 percent of employees are in long-term disability plans, but those plans generate more than 60 percent of the litigation, whereas other plans have participation by more than half of employees but account for a very small portion of the litigation that's out there," Anderson said. "What that means is, as a society, we're spending a disproportionate amount of judicial resources on resolving disputes about this one type of plan, even though it's not the most common one out there."
According to Anderson, employee benefits lawyers have long known that legal challenges to benefit denials make up a substantial number of cases litigated under the Employee Retirement Income Security Act (ERISA), the federal law that governs private employee benefits plans. But until now, there hasn't been an empirical study that deeply examined those cases, said Anderson, who studied hundreds of federal case files to gather data for the study.
The article also assessed how frequently the parties in benefits cases raised specific kinds of arguments. One such argument, that the decision maker who denied a participant's claim for benefits had a conflict of interest, was asserted more often in disability cases than in cases involving other kinds of benefit plans.
Although the study did not address the underlying reasons why plaintiffs in disability cases were more likely to assert that there was a conflict of interest, Anderson speculated that the difference might be attributable to the prominent role of insurance companies in deciding disability claims.
"It's an insurance company that administers the plan, that decides on the claim, and ultimately has to foot the bill if the benefit is granted – and that's a conflict of interest that everyone can easily see," he said.
According to the study, disability cases also were more likely to be settled than cases involving other types of plans. The study did not measure the reasons that might underlie that difference, Anderson noted.
"You could guess that since they're typically about smaller sums of money than, say, life insurance settlements, they tend to involve plaintiffs who are under more monetary pressure to settle and take something as opposed to waiting out the process and attempting to get more," he said. "So there are pragmatic litigation reasons why those cases might be more likely to settle."
One also might expect that a claim of a conflict-of-interest would make a settlement more likely, Anderson said.
"It might change the calculation for the defendants as to whether it's worth pursuing a case to the very last yard – or whether it makes more sense to just pay off the plaintiff to make the case go away," he said.
And, in fact, the article found that disability cases, in which conflict of interest claims were more common, were more likely to settle than other types of cases. But across all categories of benefits cases, those with claims of a conflict of interest were actually less likely to settle. The reasons for that are not clear, Anderson said.
He also believes an alternative to litigation that is available for most health care benefit claims could be applied to disability claims as well. Under either state law or the federal Affordable Care Act, most health plan participants whose claims are denied, instead of going to court, can choose to have an independent doctor who doesn't work for the employer or the insurance company decide whether they're entitled to the benefits.
"Because most disability claims, like health care claims, involve medical evidence, review by independent experts might be a desirable approach for disability benefits, too," Anderson said. "It would seem that that type of situation would lend itself well to independent review, so then we wouldn't have federal judges with no medical expertise reviewing decisions about whether or not someone meets the definition of disability."
Provided by University of Illinois at Urbana-Champaign