This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
Ovarian cancer: New biological markers found that may predict which patients won't respond to chemotherapy
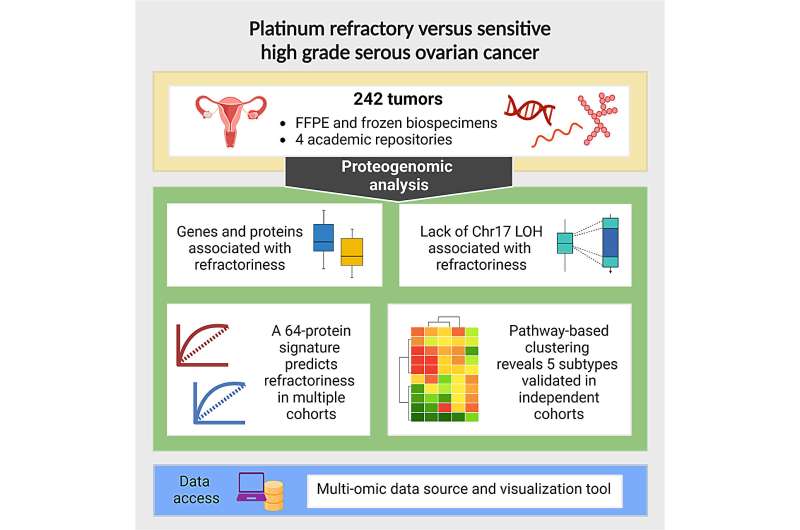
Using a novel proteogenomic strategy and a variety of machine learning tools, investigators from the Icahn School of Medicine at Mount Sinai and colleagues have identified a 64-protein signature that may predict a subset of ovarian cancer patients who are unlikely to respond to chemotherapy.
The multi-center study, published online in Cell , reports on a pioneering analysis of chemo-refractoriness in high-grade serous ovarian cancer (HGSOC). The work also implicates possible therapeutic targets for these patients. The paper is titled, "Proteogenomic analysis of chemo-refractory high-grade serous ovarian cancer."
Epithelial ovarian cancer causes over 185,000 global deaths annually. HGSOC accounts for 60% of these deaths.
Despite advances in treatment, mortality has remained the same for these patients in the past 40 years. Currently, there's no way to distinguish refractory cases (who never respond to chemotherapy), leading some patients to unnecessarily experience the adverse effects of platinum-based chemotherapy without the benefits.
"To address this critical unmet need, we performed a proteogenomic analysis to identify molecular signatures of refractory HGSOC and potential treatment targets. Predictors of chemo-refractoriness could enable precision oncology, sparing patients the toxicity and helping to identify the most effective therapy through targeted clinical trials," says Pei Wang, Ph.D., Professor of Genetics and Genomic Sciences at Icahn Mount Sinai and co-corresponding author on the paper.
The investigators studied 242 tumors samples collected from HGSOC patients comprising both chemo-refractory and chemo-responsive individuals before they received chemotherapy. Using advanced computer models to analyze protein and gene expression profiles of the tumors, they found a specific group of 64 proteins that can predict which tumors won't respond well to the first-line platinum-based therapy. This prediction was confirmed in two independent cohorts of patients.
In addition, based on pathway activity measurements derived from the proteomics data, the team also identified five new HGSOC subtypes, validated in two independent patient groups and in lab-grown tumor mouse models, suggesting that different treatment strategies may be needed.
Next, the researchers plan to confirm their findings in additional retrospective and prospective studies. Once validated, these tools, say the investigators, can be used by clinicians to design customized alternative treatments other than the current standard chemotherapy to help patients with refractory tumors.
As a part of the research, the lab of Amanda Paulovich, MD, Ph.D., a lead author of the study, is working on a new test that uses a multiplex assay panel to measure the proteins in the prediction model faster and more efficiently. Dr. Paulovich is a professor at Fred Hutchinson Cancer Center in Seattle, where she holds the Aven Foundation Endowed Chair.
The test will combine information from multiple proteins to create a single score that indicates the likelihood of chemo-refractory disease. If successful, say the investigators, it could be a significant development for about 35% of patients with ovarian cancer who could avoid treatments that won't work for their specific type of cancer.
More information: Amanda G. Paulovich, Proteogenomic analysis of chemo-refractory high grade serous ovarian cancer, Cell (2023). DOI: 10.1016/j.cell.2023.07.004. www.cell.com/cell/fulltext/S0092-8674(23)00737-7
Journal information: Cell
Provided by The Mount Sinai Hospital