Researchers develop better ways to culture living heart cells on the International Space Station
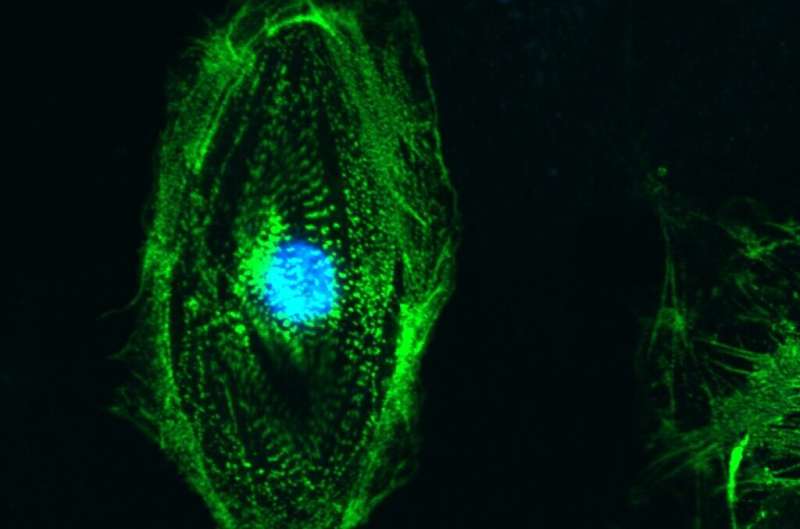
As part of preparing for an experiment aboard the International Space Station, researchers explored new ways to culture living heart cells for microgravity research. They found that cryopreservation, a process of storing cells at -80°C, makes it easier to transport these cells to the orbiting lab, providing more flexibility in launch and operations schedules. The process could benefit other biological research in space and on Earth.
The investigation, MVP Cell-03, cultured heart precursor cells on the space station to study how microgravity affects the number of cells produced and how many of them survive. These precursor cells have potential for use in disease modeling, drug development, and regenerative medicine, such as using cultured heart cells to replenish those damaged or lost due to cardiac disease.
Previous studies suggest that culturing such cells in simulated microgravity increases the efficiency of their production. But using live cell cultures in space presents some unique challenges. The MVP Cell-03 experiment, for example, must be conducted within a specific timeframe, when the cells are at just the right stage. Flight changes and crew availability could lead to delays that affect the research.
"Sometimes a flight is delayed and investigators have to prepare batches and batches of backup cells," says Chunhui Xu of Emory University School of Medicine in Atlanta, principal investigator for MVP Cell-03. "Astronauts face an overwhelming amount of work the day investigations arrive, but these cells need fresh medium right away. We thought we had better work out this procedure ahead of time."

So her lab conducted experiments on new methods for transporting and culturing the heart cells. Their results, recently published in the journal Biomaterials, show that cryopreservation does not appear to affect the cells and even offers the added benefit of protecting cells from excess gravity experienced during launch.
"Cryopreservation allows you to significantly reduce the effect of launch so that your research can look only at the effects of the low-Earth orbit environment," says Marc Giulianotti, program director for the ISS US National Laboratory, which sponsored the research. "The technique also opens up possibilities for experiments in lunar or deep space environments. It could even provide significant advantages for terrestrial research in terms of shipping cells and tissues across a country or the planet."
Xu's team also compared a new cell culture medium that does not require carbon dioxide with the current standard medium, which does, and found no difference between the two. Carbon dioxide adds weight and mass—and cost—to a space launch. The research team tested several modifications to culture media to improve cryopreservation procedures as well.
The cryopreserved heart cells flew to the space station in March 2020. Astronauts thawed and successfully cultured them, generating beating heart cells. Those were returned to Earth after 22 days of spaceflight.
"There is no reason to think you could not do this with other cell types," says Giulianotti. "It makes things much easier for investigators. They can work on their own schedule for sending cells to station without having to start the experiment as soon as the capsule gets there, when there is a mad rush to get everything done. Not having to keep cells alive on the trip reduces the footprint of the experiment and the cost of materials."
Xu says the team reported results now because they thought it would be helpful for other research in space and with this type of cell.
"We thought cryopreservation could benefit so many different applications, and can imagine many situations where a carbon dioxide-independent medium would be quite useful," Xu says.
Giulianotti calls the results a significant step for next-generation space research. "At the National Lab, we can envision banks of cell lines that you can just pull to start an experiment. It has a lot of future potential."
More information: Antonio Rampoldi et al, Cryopreservation and CO2-independent culture of 3D cardiac progenitors for spaceflight experiments, Biomaterials (2021). DOI: 10.1016/j.biomaterials.2021.120673
Journal information: Biomaterials
Provided by NASA