Unmasking a hidden killer: Successfully detecting cancer in blood of patients undergoing treatment

Pancreatic cancer is one of the most lethal cancers, but difficult to diagnose: few sufferers have symptoms until the cancer has become large or already spread to other organs. Even then, symptoms can be vague and easily misconstrued as more common conditions.
This is why Dr. Yuling Wang is so excited by results of a trial completed in late 2019, which—using plasmonic nanoparticles developed by the Centre for Nanoscale BioPhotonics (CNBP)—successfully detected signs of the cancer in blood of patients undergoing treatment. The paper was recently published in the journal American Chemical Society—Sensors.
"The test gave a very high signal in the blood for late-stage or very serious tumors, where other techniques cannot detect anything," said Dr. Wang, an associate investigator at the Centre's Macquarie University node in Sydney, in work led by Prof Nicolle Packer. "We need to test many more patient samples to validate the approach, but the strength of the signal was very encouraging."
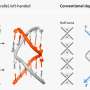
They did this by developing a method, using surface-enhanced Raman spectroscopy nanotags, that simultaneously detects three known pancreatic cancer biomarkers in blood. Known as extracellular vesicles, or EVs, they contain DNA and proteins for cell-to-cell communication and are shed from pancreatic cancer cells into surrounding body fluids. The CNBP method zeros in on three: Glypican-1, epithelial cell adhesion molecules and CD44V6.
For the experiment, biopsies of healthy donors were provided alongside those of known sufferers of pancreatic cancer, in double-blind tests where the researchers did not know which was which. Nevertheless, the blood of sufferers was easily identified. The technique was so sensitive it could spot EVs as small as 113 nanometres in diameter—or less than 1% the width of a human hair—in every millilitre of blood.
The pancreas is part of the digestive system, secreting insulin into the bloodstream to regulate the body's sugar level as well as important enzymes and hormones into the small intestine to help break down food. Pancreatic cancer is the fifth biggest cancer killer in Australia and has a 5-year survival rate of 8.7%. More than 3000 Australians are diagnosed annually, and surgery to remove the cancer is a long and complex process, requiring long hospital stays.
Because existing blood tests for the protein biomarkers of pancreatic cancer are unreliable, imaging with endoscopic ultrasound or MRI scans is necessary. Even then, anomalies can only be confirmed with a biopsy of the organ, which is invasive and ultimately relies on a trained pathologist to recognize signs of the cancer under a microscope. As a result, there's some subjectivity involved and cancer can be present but still be missed.
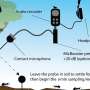
"Our approach is non-invasive—we don't need to take tissue from the patient, we just use a handheld device to test blood for targeted biomarkers, which gives a very quick result," Dr. Wang said. It may also help provide earlier diagnosis of the cancer.
While the work is a proof-of-concept, it was also able to detect colorectal and bladder cancer biomarkers—although not as clearly as those for pancreatic cancer. Nevertheless, the results are so encouraging that a commercial partner has committed funding to CNBP so it can develop a handheld spectrometer for cancer biomarkers in blood.
More information: Wei Zhang et al. Enabling Sensitive Phenotypic Profiling of Cancer-Derived Small Extracellular Vesicles Using Surface-Enhanced Raman Spectroscopy Nanotags, ACS Sensors (2020). DOI: 10.1021/acssensors.9b02377
Journal information: ACS Sensors
Provided by CNBP