Fungi found in the guts of healthy adults just travel through
Fungi found in the gastrointestinal tracts of healthy adults are largely transient and stem from the mouth or foods recently consumed, according to new research published this week in mSphere, an open access journal from the American Society for Microbiology.
"Many of the fungi most commonly detected in stool samples are also present in food or in the mouth," said lead study author Thomas A. Auchtung, Ph.D., a senior scientist at the Alkek Center for Metagenomics and Microbiome Research at Baylor College of Medicine in Houston. "To recognize which gut fungi are likely to have a sustained influence on human health, there is a need to separate transient members of the GI tract from those capable of colonizing."
Auchtung and colleagues sequenced genetic material from the stool, saliva and food of healthy adults following the consumption of different controlled diets. The only fungi they identified in DNA from the participants' stool samples were also present in their saliva and/or food, indicating that these fungi pass through the GI tract as part of digestion, rather than colonize and grow like most bacteria found in the gut. Additional laboratory experiments failed to detect any additional fungi.
There are a few reasons why fungi might not be found in the guts of healthy adults, Auchtung said: It may be that people have strong enough immune systems to keep fungi from growing, or that through recent or long-term evolution, humans have lost some fungal partners. In addition, he said, "a lot of fungi don't grow well at body temperature, and the gut can be a very inhospitable place." However, he said, because fungi can cause serious infections in immunocompromised individuals and are found at increased abundance in multiple disorders of the GI tract, "understanding normal fungal colonization is essential for proper treatment and prevention of fungal pathogenesis."
Auchtung's team conducted several experiments to study fungi in the gut. First, they looked at fungi from stool samples in adults participating in the Human Microbiome Project, a National Institutes of Health initiative to characterize microorganisms found in healthy and diseased humans. They looked at the rate in which new fungi could be detected in 148 stool samples from 100 volunteers, and found that there were more unique fungal than bacterial species. This may be because most of the fungi came from eating different foods, whereas many of the same bacteria live in the guts of different people.
Next, the team asked four healthy adult volunteers to consume the same sequence of four specific diets for about two days each: nuts and dried berries; beans, corn and rice; pasta and marinara sauce; and an egg, sausage and cheese sandwich and peas. All volunteers provided stool and saliva samples on a day of their regular diet, and after consuming the special diets. The volunteers were found to have fungi that either corresponded to species in their saliva, in foods that they frequently consumed, or in foods that were components of the experimental diets.
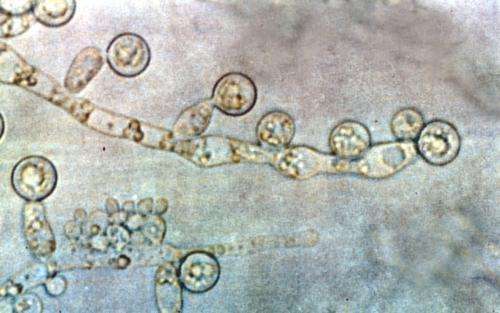
The team also injected some stool from healthy volunteers into bioreactors, lab equipment to simulate the human gut in different conditions. The only fungus identified was Candida albicans, and only in a condition of some oxygen and low bacterial diversity. Under conditions resembling a healthy gut, there was no evidence of fungal persistence.
Additionally, the team examined whether Saccharomyces, a group of fungi that can survive gastrointestinal transit and one of the most commonly detected fungi in human stool, would continue to be detected in a healthy adult following a diet free of Saccharomyces cerevisiae—a yeast common in beer, breads and processed foods—for one week. After just two days on the special diet, the amount of Saccharomyces dropped to nearly undetectable levels, suggesting it came solely from S. cerevisiae in the diet.
In a final experiment, investigators wanted to see how Candida albicans, a yeast found in the mouth that is capable of causing disease, contributed to stool samples. A couple of healthy volunteers brushed their teeth with fluoride toothpaste either once a day (at night) or after every meal. The team found 10- to 100-fold less C. albicans in the stool after they brushed with every meal, indicating that a large portion of C. albicans found in the stool derived from the mouth.
Provided by American Society for Microbiology