An improved anti-addiction medication
Drug addiction continues to plague vast numbers of people across the world, destroying and ending lives, while attempts to develop more effective pharmaceutical addiction treatments continue. Scientists now report in the Journal of the American Chemical Society the development of a potent new medicine to fight addiction, which might also be an effective treatment for epilepsy and other conditions.
Vigabatrin is an anti-epilepsy medication approved by the Food and Drug Administration that has also been shown to be effective against addiction to cocaine, nicotine, methamphetamine, heroin and alcohol in animal models. In humans, vigabatrin eliminates cocaine addiction in 28 percent of patients. It works by blocking an enzyme, γ-aminobutyric acid (GABA) aminotransferase, which breaks down GABA. The result is higher levels of this neurotransmitter in the brain and diminished narcotic-activated release of dopamine. Long-term vigabatrin therapy can have serious side effects however, causing eye damage in up to 40 percent of those treated. So, Richard B. Silverman, Stephen L. Dewey and colleagues wanted to develop a more potent inhibitor of GABA aminotransferase with fewer side effects.
In previous work, the researchers designed a compound, CPP-115, that is 186 times more efficient in inactivating GABA aminotransferase than vigabatrin. In this study, they used computational molecular dynamics simulations of CPP-115 in complex with the enzyme to develop a new and improved agent with 10 times greater efficiency. The drug should also be less likely to cause side effects, as it has fewer off-target activities in in vitro tests. In initial rat experiments, the new compound was far better at blocking dopamine release after a cocaine or nicotine stimulus than CPP-115. The researchers say that future work could examine whether the computational approach could be generalized to improve other mechanism-based enzyme inhibitors in the laboratory before testing them on animals.
More information: Jose I. Juncosa et al. Design and Mechanism of (S)-3-Amino-4-(difluoromethylenyl)cyclopent-1-ene-1-carboxylic Acid, a Highly Potent γ-Aminobutyric Acid Aminotransferase Inactivator for the Treatment of Addiction, Journal of the American Chemical Society (2018). DOI: 10.1021/jacs.7b10965
Abstract
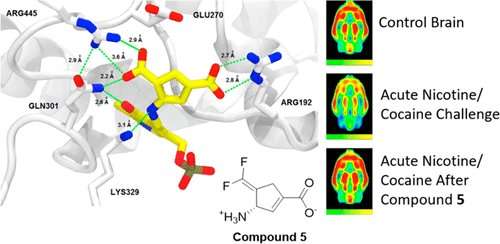
γ-Aminobutyric acid (GABA) is the major inhibitory neurotransmitter in the central nervous system. Inhibition of GABA aminotransferase (GABA-AT), a pyridoxal 5′-phosphate (PLP)-dependent enzyme that degrades GABA, has been established as a possible strategy for the treatment of substance abuse. The raised GABA levels that occur as a consequence of this inhibition have been found to antagonize the rapid release of dopamine in the ventral striatum (nucleus accumbens) that follows an acute challenge by an addictive substance. In addition, increased GABA levels are also known to elicit an anticonvulsant effect in patients with epilepsy. We previously designed the mechanism-based inactivator (1S,3S)-3-amino-4-difluoromethylenyl-1-cyclopentanoic acid (2), now called CPP-115, that is 186 times more efficient in inactivating GABA-AT than vigabatrin, the only FDA-approved drug that is an inactivator of GABA-AT. CPP-115 was found to have high therapeutic potential for the treatment of cocaine addiction and for a variety of epilepsies, has successfully completed a Phase I safety clinical trial, and was found to be effective in the treatment of infantile spasms (West syndrome). Herein we report the design, using molecular dynamics simulations, synthesis, and biological evaluation of a new mechanism-based inactivator, (S)-3-amino-4-(difluoromethylenyl)cyclopent-1-ene-1-carboxylic acid (5), which was found to be almost 10 times more efficient as an inactivator of GABA-AT than CPP-115. We also present the unexpected crystal structure of 5 bound to GABA-AT, as well as computational analyses used to assist the structure elucidation process. Furthermore, 5 was found to have favorable pharmacokinetic properties and low off-target activities. In vivo studies in freely moving rats showed that 5 was dramatically superior to CPP-115 in suppressing the release of dopamine in the corpus striatum, which occurs subsequent to either an acute cocaine or nicotine challenge. Compound 5 also attenuated increased metabolic demands (neuronal glucose metabolism) in the hippocampus, a brain region that encodes spatial information concerning the environment in which an animal receives a reinforcing or aversive drug. This multidisciplinary computational design to preclinical efficacy approach should be applicable to the design and improvement of mechanism-based inhibitors of other enzymes whose crystal structures and inactivation mechanisms are known.
Journal information: Journal of the American Chemical Society
Provided by American Chemical Society



















