Clinical tests show that biosensors could pave the way for a personalized antibiotherapy in the future
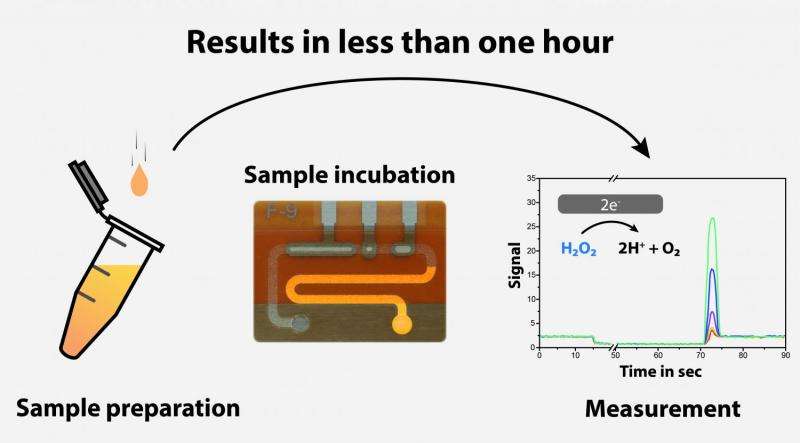
Personalized drug therapy adjusting the dose, dosage intervals, and the duration of treatment to fit individual patients' needs is increasingly important. Frequently, medications are dosed in such a way that each patient receives the same standardized amount of a drug. Thus, clinical conditions such as overall state of health, metabolism, or other physical factors are often not sufficiently considered. A research team at the University of Freiburg has developed a bioanalytical method to measure the class of β-lactam antibiotics in human blood onsite – in the operating room, intensive ward or doctor's office, or even the patient's home. "This way, we can easily determine just how quickly the human body metabolizes a drug," said the microsystems engineer Dr. Can Dincer, who is the head of the research team.
The researchers recently published their results in the journal Scientific Reports.
This new method makes it possible to individually adjust the necessary dose of a medication for each patient. "We've proven the applicability of our system for a personalized antibiotherapy by on-site monitoring the clearance of drugs in two patients who were treated with ß-lactam antibiotics undergoing surgery," Dincer said. "Based on these results, our next step will be to perform a quantitative cohort study that will determine the usefulness of personalized antibiotherapy," he added.
At the end of 2016, the research team presented its biosensor technology allowing the rapid and simultaneous monitoring of different antibiotics in human blood (www.pr.uni-freiburg.de/pm/2016/pm.2016-11-14.159). In their recently published study, the scientists further developed their system by implementing another natural sensor protein that can quantify β-lactam antibiotics. In human medicine, β-lactam antibiotics are often used to prevent and treat infectious diseases.
More information: R. Bruch et al. Clinical on-site monitoring of ß-lactam antibiotics for a personalized antibiotherapy, Scientific Reports (2017). DOI: 10.1038/s41598-017-03338-z
Journal information: Scientific Reports
Provided by Albert Ludwigs University of Freiburg