Colour-changing burns dressing will help fight against antibiotic resistance
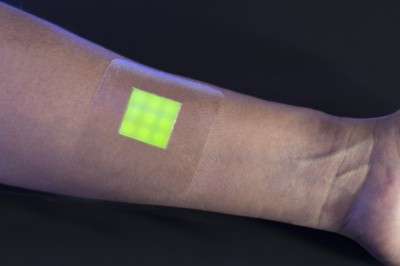
A 'smart' medical dressing, developed by our scientists, that changes colour when it detects infection will improve treatments for burns patients and help combat the global problem of antibiotic resistance by reducing the unnecessary use of antibiotics.
Children with burn wounds are particularly susceptible to bacterial infections because of their immature immune systems. Such infections can slow wound healing, leading to longer hospital stays as well as increased risk of permanent scarring. In severe cases, burn infection can lead to sepsis, which can kill.
It is currently extremely difficult for doctors to diagnose infections quickly and at the patient's bedside. Existing methods take up to 48 hours and require removing the wound dressing which is painful and distressing for the patient and may result in slower healing and potentially life-long scarring. Due to this time delay, when a child with a burn shows symptoms of a possible infection, the clinician often has to treat them with antibiotics as a precaution before their infection is confirmed.
However, treatment with antibiotics when there is no infection can lead to bacteria becoming resistant to antibiotics. Antibiotic resistance has been identified by world leaders as one of the biggest health threats we face today.
Colour-changing dressing
Scientists from the Department of Chemistry, in collaboration with the Healing Foundation Children's Burns Research Centre, based at the Bristol Children's Hospital, and the University of Brighton have developed a prototype dressing that will change colour as soon as the wound is infected.
This will enable doctors to quickly treat only those patients with an infection, without giving unnecessary antibiotics to patients who may simply have symptoms due to a cold.
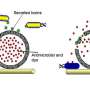
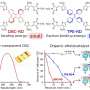
Dr Toby Jenkins, Reader in Biophysical Chemistry at Bath leading the project, explained: "Our medical dressing works by releasing fluorescent dye from nanocapsules triggered by the toxins secreted by disease-causing bacteria within the wound.

"The nanocapsules mimic skin cells in that they only break open when toxic bacteria are present; they aren't affected by the harmless bacteria that normally live on healthy skin.
"Using this dressing will allow clinicians to quickly identify infections without removing it, meaning that patients can be diagnosed and treated faster. It could really help to save lives."
Taking research from the lab to the clinic
The team has been awarded almost £1 million by the Medical Research Council, through the Biomedical Catalyst funding stream, to test the responsiveness of the prototype dressing to samples taken from the wounds of burns victims.
Dr Jenkins commented: "Translating research from the laboratory towards the clinic is fraught with complexity, but this award will allow us to start this critical translational pathway. Working with our industry partner, the funding will be used to design, manufacture and package a final prototype dressing, safe and ready for trial in humans."
Dr Amber Young is the Clinical Lead for the Healing Foundation Children's Burns Research Centre at Bristol Children's Hospital. She will be taking wound swabs and blister fluid from young burns patients and linking these to patients' symptoms for Dr Jenkins to test how well the new dressing detects infection in samples from real patients.
She said: "Children are at particular risk of serious infection from even a small burn. However, with current methods clinicians can't tell whether a sick child might have a raised temperature due to a serious bacterial burn wound infection, or just from a simple cough or cold.
"Being able to detect infection quickly and accurately with this wound dressing will make a real difference to the lives of thousands of young children by allowing doctors to provide the right care at the right time, and also, importantly, reduce the global threat of antibiotic resistance."
Understanding how infections take hold
Dr Brian Jones, Reader in Molecular and Medical Microbiology from the University of Brighton, will be coordinating work to understand and optimise how the dressing responds to problematic bacteria in wounds, and also to collect samples from adult patients at Queen Victoria Hospital in West Sussex.
Dr Jones added: "This new dressing technology will not only help clinicians provide the best possible treatment for patients with burns, but could also tell us a lot about how wound infections begin and how they affect the normal healing process. This could in turn lead to even further advances in treating these infections."
Once the dressing has been proven to effectively detect infection in swab samples from patients, the team plans to work with healthcare company Hartmann to develop the dressing for use in hospitals in around four years.
Provided by University of Bath