Discovery of how bacteria survive antibiotics may improve treatment of infectious diseases
Infectious diseases kill more people worldwide than any other single cause, but treatment often fails because a small fraction of bacterial cells can transiently survive antibiotics and recolonize the body. A study published June 4 in Molecular Cell reveals that these so-called persisters form in response to adverse conditions through the action of a molecule called Obg, which plays an important role in all major cellular processes in multiple bacterial species. By revealing a shared genetic mechanism underlying bacterial persistence, the study paves the way for novel diagnostic tools and more effective treatment strategies for a range of bacterial infections.
"Persisters pose a fundamental hurdle to the treatment of chronic and biofilm infections by bacterial and fungal pathogens," says co-senior study author Jan Michiels of KU Leuven - University of Leuven. "Our findings suggest that combining antibiotic treatment with a therapy specifically targeting the novel persistence pathway we discovered would prove advantageous by enhancing patient responses to antibiotic treatment and by shortening antibiotic therapy duration."
Persistence is triggered in part by bacterial toxins that shut down critical cellular processes, such as protein synthesis or energy production, forcing the bacterial cells to enter a dormant state in which they are no longer susceptible to killing by antibiotics. But the mechanisms underlying toxin-mediated persistence have not been clear, and little is known about how environmental signals trigger bacterial persistence.
To answer these questions, Michiels and his team focused on the potential role of Obg because this enzyme is at the nexus of major cellular processes, such as protein and DNA synthesis, and it triggers dormancy when cellular energy levels are low. They found that high levels of Obg protected nutrient-starved intestinal bacteria called Escherichia coli and the pathogen Pseudomonas aeruginosa from two antibiotics that interfere with DNA and protein synthesis. "This indicates that a common mechanism to produce persisters is active in different bacterial species," Michiels says. "Therefore, Obg could be a target for the development of novel therapeutics against infectious diseases."
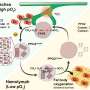
Obg induced persistence in E. coli by increasing levels of a toxic molecule called HokB, which causes small holes to form in the bacterial membrane, thereby halting energy production and triggering dormancy. However, deletion of hokB did not decrease persistence in E. coli, and this gene was absent in P. aeruginosa, suggesting that persistence is controlled by at least one other Obg-regulated pathway waiting to be discovered. Another question for future research is how persistent cells can recover from toxin-induced damage and switch back to the normal, non-persistent state. "Answering these fundamental questions will pave the way for translational research that could ultimately lead to better therapies to combat bacterial infections."
More information: Molecular Cell, Verstraeten et al.: "Obg and membrane depolarization are part of a microbial bet-hedging strategy that leads to antibiotic tolerance" dx.doi.org/10.1016/j.molcel.2015.05.011
Journal information: Molecular Cell
Provided by Cell Press