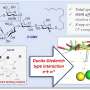
Scientists model the pathways of pain-blocking meds
Benzocaine, a commonly used local anesthetic, may more easily wiggle into a cell's membrane when the membrane is made up of compounds that carry a negative charge, a new study shows. The finding could help scientists piece together a more complete understanding of the molecular-level mechanisms behind pain-blocking medicines, possibly leading to their safer and more effective use.
Most scientists believe that local anesthetics prevent pain signals from propagating to the central nervous system by blocking nerve cells' sodium channels, but exactly how the medicines accomplish this feat remains vague. Since the solubility of anesthetics in the cell membrane can affect the medicine's potency, some scientists have hypothesized that certain anesthetics may block the action of sodium channels indirectly, by entering the cell membrane and jostling the channels into a new shape that prevents ion flow.
With the aim of further investigating such complex processes, scientists from the Universidad Politecnica de Cartagena in Spain and the Universidad Nacional de San Luis in Argentina have created a computer model that calculates the probability of molecules of benzocaine entering a cell's membrane, based on the composition of the membrane.
As reported in the AIP's Journal of Chemical Physics, the model predicts that membranes made of a large percentage of DPPS, a negatively charged phospholipid component of cells, present less of a barrier to benzocaine molecules than membranes made mostly of DPPC, a neutral phospholipid. DPPS is normally found as one of the main components of cell membranes in the central nervous system, as well as a component of the inner side of membranes in other humans cells.
More information: "Thermodynamic study of benzocaine insertion into different lipid bilayers" is accepted for publication in the Journal of Chemical Physics.
Provided by American Institute of Physics