Overcoming Drug Resistance—Nanoparticles Trigger Built-In Cell-Death Signal
One of the most vexing problems in treating cancer is the propensity of tumors to develop resistance to a wide range of anticancer drugs. Over 70 percent of ovarian cancer patients, for example, have drug-resistant tumors at the time of their initial diagnosis, and virtually all patients who relapse have drug-resistant tumors.
Researchers have identified the major mechanisms that cancer cells use to neutralize the cytotoxic, or cell-killing, effects of anticancer drugs, and now they are using nanotechnology to help derail drug resistance and improve the odds of successfully treating cancer.
In one recently published paper, Mansoor Amiji, Ph.D., principal investigator of a National Cancer Institute (NCI)-funded Cancer Nanotechnology Platform Partnership at Northeastern University, and his collaborators have demonstrated that the combination of the anticancer drugs paclitaxel and tamoxifen, delivered to tumors in polymer-based nanoparticles, overcomes multiple drug resistance in a mouse model of human ovarian cancer.
This paper, which appears in the journal Clinical Cancer Research, describes experiments showing that tamoxifen, when delivered into a tumor cell by the polymer nanoparticle, acts to boost the intracellular level of a fatty molecule known as ceramide, which in turn allows the nanoparticle-delivered paclitaxel to trigger apoptosis, or programmed cell death.
After initial experiments with drug-resistant human ovarian cancer cells showed that a combination of tamoxifen- and paclitaxel-loaded nanoparticles triggered substantial cell death in the resistant cells, the investigators treated tumor-bearing animals with the two nanoparticles. Three weeks after treatment, tumors were one-third the size of those in animals that received no treatment or treatment with paclitaxel alone. Administration of a second dose produced further significant tumor growth suppression. These studies also showed that the combined nanoparticle treatment was accompanied by few adverse side effects.
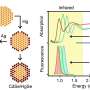
Taking a slightly different approach, Gavin Robertson, Ph.D., and his colleagues at the Pennsylvania State University College of Medicine used nanoparticles to deliver ceramide itself to cancer cells, which also appears to overcome drug resistance. In a paper also published in Clinical Cancer Research, Dr. Robertson’s team treated melanoma and breast cancer cells with the anticancer agent sorafenib, which has been approved to treat kidney and liver cancer, together with ceramide encapsulated in a nanoscale liposome. Nanoparticle encapsulation enables ceramide to cross the cell membrane and enter a cell’s cytoplasm.
Previous clinical trials with sorafenib failed to demonstrate therapeutic efficacy in treating melanoma or breast cancer. However, the combination of sorafenib and nanoparticle-encapsulated ceramide had a marked toxic effect on both melanoma cells and breast cancer cells growing in culture. When administered to animals with human melanoma or breast tumors, the combination therapy produced a significant reduction in tumor growth with few if any apparent side effects.
Working with the Penn State group, Scott McNeil, Ph.D. and his colleagues at the NCI’s Nanotechnology Characterization Laboratory (NCL) have been studying how liposomal ceramide behaves in the body. The initial results of these studies, which were conducted as part of a larger effort whose goal is to develop nanoparticulate ceramide for human clinical trials, appear in the journal Drug Metabolism and Disposition.
Using tritium-labeled nanoparticles loaded with carbon-14 labeled ceramide, the NCL team was able to trace the fate of both the nanoparticles and their payload when injected into rats. The results of this study showed that while the lipid-based nanoparticles largely remained in circulation, they were able to deliver their ceramide payload into cells. The most likely mechanism for intracellular delivery involved exchange of ceramide from the lipid-bilayer of the nanoparticles to the lipid-bilayer of tumor cells. The results of this exchange process led to rapid tissue distribution of ceramide without apparent adverse effects, despite the fact that a substantial amount of ceramide escapes from the liposomes before reaching the tumor.
To overcome this “leakage,” Yechezkel Barenholz, Ph.D., and his collaborators at the Hebrew University-Hadassah Medical School in Jerusalem added a lipid-polymer construct to liposomes intended to encapsulate ceramide. The resulting nanoparticles were far more stable than standard liposomes. As a result, these liposomes were able to deliver larger doses of ceramide to tumor cells, increasing the therapeutic efficacy of ceramide administration. The resulting liposomes were also more stable when stored, a useful characteristic should such a formulation eventually receive regulatory clearance for use in humans.
The work from Dr. Amiji’s group, which was supported by the NCI’s Alliance for Nanotechnology in Cancer, is detailed in the paper “Modulation of Drug Resistance in Ovarian Adenocarcinoma by Enhancing Intracellular Ceramide Using Tamoxifen-Loaded Biodegradable Polymeric Nanoparticles.” Investigators from the Massachusetts General Hospital also participated in this study.
The work from Dr. Robertson and his collaborators is described in the paper “Combining Nanoliposomal Ceramide with Sorafenib Synergistically Inhibits Melanoma and Breast Cancer Cell Survival to Decrease Tumor Development.” Investigators from the Foreman Foundation for Melanoma Research and the Medical University of South Carolina also participated in this study.
The work from Dr. McNeil and his collaborators, which was supported by the NCI’s Alliance for Nanotechnology in Cancer, is detailed in the paper “Rapid Distribution of Liposomal Short-Chain Ceramide In Vitro and In Vivo.” Investigators from the Penn State College of Medicine also participated in this study.
The work from Dr. Barenholz’s group is detailed in the paper “Physicochemical and Biological Characterization of Ceramide-Containing Liposomes: Paving the Way to Ceramide Therapeutic Application.”
Source: National Cancer Institute