Stealth technology maintains fitness after sex
Pathogens can become superbugs without their even knowing it, research published today in Science shows. 'Stealth' plasmids - circular 'DNA parasites' of bacteria that can carry antibiotic-resistance genes - produce a protein that increases the chances of survival and spread of the antibiotic-resistant strain.
Low-cost plasmids, described for the first time in the study are a threat to use of antibiotics.
Plasmids are naturally occurring 'DNA parasites' of many bacterial species and have been known about for over 30 years. Some are able to transfer themselves from one bacterial cell to another through a sex-like process called conjugation, contributing to bacterial evolution. Worryingly, as well as copying themselves plasmids can pick up and transfer bacterial genes, such as those that make pathogens resistant to antibiotics.
However, the plasmid comes at a cost to the host bacterium: gaining a plasmid can reduce the host's ability to grow and reduce its fitness. When antibiotic treatment is stopped, the new microbe–plasmid combination will be eliminated quickly through fierce competition from more 'fit', plasmid-free bacteria.
The research teams, led by Professor Charles J. Dorman at Trinity College Dublin, Ireland, and Dr John Wain at the Wellcome Trust Sanger Institute in Cambridge, UK, have discovered that an important class of plasmids use a stealth gene (called sfh) to allow entry into a new bacterium with minimal reduction in fitness.
With the low-cost version of the resistance plasmid they have described in Salmonella, resistant bacteria are likely to survive and the resistance genes to persist even if antibiotic therapy is stopped.
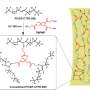
Their research shows that sfh codes for a protein that is very similar to another bacterial protein: the role of the protein is to organise the genetic material in bacterium and control activity of many genes, including those involved in causing disease. The sfh protein binds to the new plasmid DNA, preventing its detection by the bacterium.
"The bacterial protein, called H-NS, is a very important molecule and affects the way a bacterial pathogen operates. By bringing in its own supply of the H-NS-like stealth protein (called Sfh), the plasmid avoids interfering with the natural balance of H-NS and DNA in the cell," explained Professor Dorman.
"Our work suggests that bacterial fitness can be manipulated by altering the proportions of H-NS and DNA in the cell, perhaps through the use of drugs, an insight that may be exploited in the future to prevent or to fight infection."
Bringing its own supply of the host-like protein is clearly an advantage for the plasmid, suggesting that the normal supply of H-NS in the bacterium may become limited when new DNA is imported. If a modified plasmid, lacking the sfh gene, is transferred to Salmonella, the effects of the plasmid are very rapidly detected.
Bacteria can acquire and transfer resistance genes through a variety of methods, but this new study shows how a single gene has the potential to increase dramatically the chance of successful - and health-threatening - transfer and survival of a battery of antibiotic-resistance genes.
The consequences for managing disease - especially in developing countries - are significant, explained Dr John Wain: "These plasmids are found in many pathogenic bacteria including those that cause typhoid and paratyphoid fever. Both of these diseases are increasing in the developing world and in the UK we are seeing more and more imported cases.
"But understanding is not enough: we now need to exploit this information to try to prevent the plasmid spreading any further."
Source: Wellcome Trust Sanger Institute