Researcher takes a muscular approach to robotics

During his childhood in Korea, Yong-Lae Park developed a love for robotics, using the nuts, bolts and metal bars from science kits to build mechanical versions of his favorite cartoon characters.
"Robotics is very interesting and attractive because you build it and it moves on its own," Park said.
Today, Park, an associate professor at Carnegie Mellon University's Robotics Institute, retains his childhood passion but directs it toward more mature creations. He's part of a team that has designed a robotic device to restore movement for sufferers of neuromuscular disorders that affect the foot and ankle, such as cerebral palsy, multiple sclerosis and drop foot.
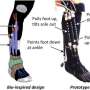
The device, which looks like a sock made of cybernetic muscle sinews, uses pneumatics to augment the strength of patients' ankles. While most such devices are bulky, this one eschews a rigid exoskeleton in favor of more nimble materials that could allow more flexibility.
Park's role in the eight-member team was to create the mechanical design and synchronize it with the muscle motions of the patient, said Bor-rong Chen, who worked on the device with Park while they studied at Harvard.
"He's a brilliant maker in general, with a very strong background in using the right material to solve a mechanical problem and designing the structure of the material," Chen said.
To design the device - a three-year effort funded by Harvard's Wyss Institute for Biologically-Inspired Engineering and the National Science Foundation - Park had to delve outside his robotic comfort zone, educating himself on the biology of the ankle. It was tough - "High school biology is my only biology background," he said.
Most exoskeletons treat the ankle as if it has only one range of motion, up and down, Park said. But when he studied the joint he realized that its movement was much more complicated. To mimic natural ankle movements, the device would have to account for this complexity.
After this realization, Park set about the formidable task of translating those complex movements into mechanical processes.
"My job is engineering, so I try to simplify those things as much as possible," Park said.
The project encountered several other challenges in its development, Park and Chen said. They had trouble determining which material to use for the actuator - an artificial muscle that mimics human movement by contracting and expanding. Building a gadget to sense the patient's movement was also difficult.
The decision to use lighter material also caused problems. Park had a hard time transferring force through the soft materials. Other, bulkier exoskeletons have more well-defined joints, allowing for easier distribution of force, but in this case the skin itself must take on the burden.
Another problem is the interaction of the device with the patient's skin. If it exerts too much pressure on a small area, it could cause discomfort. Park is working on making the distribution of pressure more uniform.
Even more obstacles lie ahead. For the device to work in an uncontrolled environment - an uneven sidewalk, versus the smooth floor of a testing lab - will require a lot of tinkering. The researchers also hope to make the device's electronics and its pneumatic power system more compact.
After those challenges are overcome, the device will still have to endure human testing. Asked when the device will hit the market, Park laughed.
"I don't know," he said. "It's hard to predict."
Chen was also reluctant to offer an estimate. After some needling, he predicted it would be three to five years before it's available to the public.
The price of the device is hard to determine so early in its development, the two colleagues said. Some aspects of its design, such as its sensors and pneumatic system, are so specialized that they will be costly to manufacture. If the device is mass-produced, it could cost between $5,000 and $10,000, Chen estimated.
The researchers envision applications for the device above the ankle. Its system of detecting and strengthening movement could be applied almost anywhere on the body, they say. Park envisions it helping elderly people with weakened muscles.
"The sensor is general enough to use to measure joint movement on the knee, elbow, ankle, wrist, even non-human movement," Chen said.
Park, who lives with his wife and daughter in Pittsburgh's Shadyside, came to the United States in 2000 to study as an undergraduate at Kansas University. He went on to earn his master's and Ph.D. in mechanical engineering at Stanford. While studying for his doctorate, he indulged his robotic obsession by researching how to better locate the positions of mechanically controlled needles during MRIs.
He plans on staying in Pittsburgh for a while, and he has big plans for his research here. His next idea is to build a remote-controlled surgical robot that is compatible with MRIs.
Looking even further into the future, Park imagines a world in which robots are intelligent enough to work alongside humans, aware not only of their presence but also of their intentions.
Whether he will see this in his lifetime, he isn't sure.
"I hope so," he said.
©2014 Pittsburgh Post-Gazette
Distributed by MCT Information Services