New tool to help surgeons remove more cancer tissue during brain surgery
Scientists are reporting development and successful initial testing of a new tool that tells whether brain tissue is normal or cancerous while an operation is underway, so that surgeons can remove more of the tumor without removing healthy tissue, improving patients' survival. The report appears in Analytical Chemistry.
Zoltán Takáts and colleagues point out that cancer can recur if tumor cells remain in the body after surgery. As a precaution, surgeons typically remove extra tissue surrounding a breast, prostate and other tumors in the body. But neurosurgeons face severe limitations because removing extra tissue can impair the patient's memory, mobility and other vital functions. Neurosurgeons thus strive to precisely identify the tumor margins during brain surgery. Current methods take too long and are unreliable. To overcome these challenges, the researchers developed a new tool that can identify the margin between cancerous and healthy tissue in half the time previously needed.
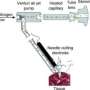
They describe linking a mainstay surgical tool termed an ultrasonic aspirator — used to break up and suction tissue — to a modified version of a standard laboratory tool called a mass spectrometer. Their tests proved successful on human brain samples. "Besides brain surgery, the method has application potential in the field of the surgery of organs including liver, pancreas or kidney," say the researchers.
More information: Real Time Analysis of Brain Tissue by Direct Combination of Ultrasonic Surgical Aspiration and Sonic Spray Mass Spectrometry, Anal. Chem., 2011, 83 (20), pp 7729–7735. DOI: 10.1021/ac201251s
Abstract
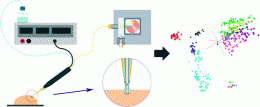
Direct combination of cavitron ultrasonic surgical aspirator (CUSA) and sonic spray ionization mass spectrometry is presented. A commercially available ultrasonic surgical device was coupled to a Venturi easy ambient sonic-spray ionization (V-EASI) source by directly introducing liquified tissue debris into the Venturi air jet pump. The Venturi air jet pump was found to efficiently nebulize the suspended tissue material for gas phase ion production. The ionization mechanism involving solely pneumatic spraying was associated with that of sonic spray ionization. Positive and negative ionization spectra were obtained from brain and liver samples reflecting the primary application areas of the surgical device. Mass spectra were found to feature predominantly complex lipid-type constituents of tissues in both ion polarity modes. Multiply charged peptide anions were also detected. The influence of instrumental settings was characterized in detail. Venturi pump geometry and flow parameters were found to be critically important in ionization efficiency. Standard solutions of phospholipids and peptides were analyzed in order to test the dynamic range, sensitivity, and suppression effects. The spectra of the intact tissue specimens were found to be highly specific to the histological tissue type. The principal component analysis (PCA) and linear discriminant analysis (LDA) based data analysis method was developed for real-time tissue identification in a surgical environment. The method has been successfully tested on post-mortem and ex vivo human samples including astrocytomas, meningeomas, metastatic brain tumors, and healthy brain tissue.
Provided by American Chemical Society