Thwarting deadly heart blockages with organic nanoparticles

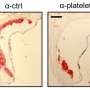
Cardiovascular disease, which kills one Australian every 12 minutes, is caused by a hardening of the arteries due to abnormal deposits of fat and cholesterol (known as plaque) in the inner lining of the artery; a process known as atherosclerosis. When plaque deposits rupture, this can cause heart attacks and stroke. But what if the plaque could be prevented from rupturing using microscopic nanoparticles?
That's the potential of exciting new organic nanoparticles first developed in Canada for cancer diagnosis and treatment. Now, researchers at the Centre for Nanoscale BioPhotonics (CNBP) are exploring how these nanoparticles could be used to identify and disarm unstable plaque deposits.
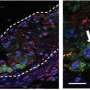
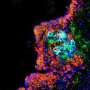
"These particles have been used in detecting and treating tumors, but we suspect they can be used for vascular health, for detection and treatment of atherosclerosis," said Victoria Nankivell, a Ph.D. student at the CNBP partner organization, the South Australian Health and Medical Research Institute, in Adelaide. "There are some unique characteristics of this nanoparticle that make it suitable for targeting key cells in atherosclerosis, such as macrophages, a key cell type found in atherosclerotic plaque."
Macrophages are a type of white blood cell of the immune system that engulfs and digests cellular debris and foreign material, such as microbes. Macrophages, in particular, produce small proteins, known as cytokines, that encourage inflammatory immune responses, enlarging the plaque and making it more likely to rupture.
Once the plaque has ruptured, this leads to blockages in the blood vessels that feed the heart, causing a heart attack; or vessels that feed the brain, causing a stroke.
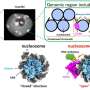
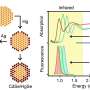
The new nanoparticles, known as porphysomes, are organic nanoparticles invented by Prof Gang Zheng, a partner investigator of the CNBP based at University of Toronto's University Health Network. Used to detect and accurately map cancer tumors, they can also be easily tracked with low-light fluorescence and have large cores which can be loaded with drugs and other agents.
Porphysomes are based on a protein that's found in high density lipoproteins, or HDLs, known as "good cholesterol." HDLs are known to limit the inflammatory processes that underlie atherosclerosis by interrupting plaque creation at several key stages.
Dr. Christina Bursill, CNBP's chief investigator of vascular health based at the University of Adelaide node, and Nankivell's supervisor, had a hunch porphysomes might also have anti-inflammatory effects in atherosclerosis. She started a collaboration with Prof Zheng's group to test out the idea. And she was right.
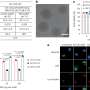
"We've now shown in culture that porphysomes do have anti-inflammatory effects in atherosclerotic plaques," said Nankivell. "When we stimulate macrophages with an inflammatory stimulus, these particles reduce the inflammatory response in those macrophages.
"We've also shown that the particles can increase the removal of cholesterol from macrophages—that's something that HDL also does," she added. "We don't quite know what it is about the porphysomes that are making it anti-inflammatory, so we want to investigate that further."
Porphysomes can also carry short-lived radioactive nuclides for extremely accurate tracking. Hence, Bursill's team plans use them to detect and track the progression of atherosclerosis in mice, to understand how the nanoparticles have their effect. For this, they are collaborating with the Baker Heart and Diabetes Institute in Melbourne, which has bred experimental mice that can be induced to develop atherosclerosis that closely resembles the plaque instability that leads to plaque rupture in humans.
Provided by Centre for Nanoscale BioPhotonics