The math behind the COVID-19 modeling

Some of us might have been happy to leave mathematics behind in high school or college, but as the COVID-19 pandemic has spread, math has had a daily effect on all of our lives—even if we don't have to crunch the numbers ourselves.
Mathematical models—built on a foundation of calculus, statistics and probability theory—have been one of the driving forces behind policies, at least in Ohio, around the COVID-19 pandemic.
"The hospitals need to know, roughly, do we have enough beds, do we have enough ventilators, and if you don't have some estimate of that you're really playing with fire," said Joe Tien, associate professor of mathematics at Ohio State and a leader on the COVID-19 modeling team. "We're still not going to say our estimates are what's going to happen but at least you have some process by which you derive an estimate; otherwise, you're completely guessing."
Ohio State has a team that has been modeling the COVID-19 pandemic since early March. It is jointly led by Tien and Greg Rempala, a professor of biostatistics in the College of Public Health, and includes researchers who study geography, medicine, environmental health and others. The team has been among the group of scientists, along with officials from the Ohio Department of Health and the Ohio Hospital Association, offering modeling and statistics to the governor's pandemic task force.
The modeling that has been used by the Ohio State team started a few years ago, long before this particular coronavirus ever jumped from animals to humans. In 2015, in response to the ongoing Ebola outbreak in West Africa, Tien, Rempala and another researcher in the Ohio State Mathematical Biosciences Institute (MBI) decided to study the ways diseases spread on human networks—between co-workers, among friends, from children to parents.
One way to study that spread: a mathematical concept known as a stochastic process, a way to analyze random happenings over time. The researchers realized that they could apply basic calculus to that process when considering disease spread and come up with a set of differential equations to study the rate of change of the number of people susceptible to the disease in a given population.
"This is where your calculus comes in—the rate of change of the number of susceptible people in the population, and that is the underlying base of the model we're looking at for COVID," Tien said. "From there, our colleagues have developed some nice statistical techniques for using statistics to find the probability of how fast the disease will spread."
The model Rempala and Tien have used, first for the Ebola outbreak and now for the COVID-19 pandemic, is an amped-up version of a model developed in the early 1900s to model the 1918-19 influenza epidemic. That model, called an SIR model, attempts to analyze the ways people interact to spread illness. "SIR" stands for "susceptible, infectious, recovered," and is a way of grouping people: Susceptible people haven't gotten an illness yet; infectious are currently infected. Recovered are those who've had the illness and survived.
An SIR model relies on data about a given disease and how it spreads, but when a disease is new—the "novel" part of "novel coronavirus" in the case of our current pandemic—reliable data can be hard to come by. And a traditional SIR model also doesn't take into account behavioral and policy changes like social distancing and stay-at-home orders.
The model that Tien and Rempala are using does.
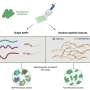
"The model had this feature that allowed these networks to get disrupted or disconnected," said Rempala. "We didn't call it social distancing—we called it a drop-out rate. And we assumed we had this network where people were interacting with each other and then stopped—they dropped out of the network. And that allowed us to model what might happen to the disease spread."
The model was limited at first by a lack of good data—and still is, to some extent. Because testing for the virus has been minimal—only a small percentage of the population has been tested, and generally only when a person is very sick—the model can't say with certainty what percentage of the population is susceptible, infectious or recovered.
But because the virus had already played out in China, Italy, South Korea and other places by the time it reached the United States, the modelers had some clues. And another type of math—simple addition and subtraction—became important. The state's hospitals had finite numbers of hospital beds, ventilators and personal protective equipment, things that were critical to being able to treat COVID-19 patients.
"Even with this limited information, we have some idea about how it expands, and that turned out to be exactly the type of information you need to make predictions about the number of hospital beds you will need," Rempala said. "With this type of approach, you cannot use it to calculate the total number of infected people in Ohio, but you can help the state plan for how much capacity it will need."
Computational equations do not equate to policies. They simply offer models showing the most educated guess, based on the best available data, of what might happen under different scenarios. In early March, when modelers first put COVID-19 figures into their equations, there were no social distancing measures. Schools, restaurants and hair salons were still open.
The initial models showed very high numbers of COVID-19 patients; after state policymakers issued stay-at-home orders and closed schools and many businesses, the models—and the real-time data of those who were sick—showed those numbers dropping.
As Ohio and other states begin to reopen, slowly in some cases, the models are still running. Those models should give policymakers some insight into how their decisions might play out in the real world.
Provided by The Ohio State University