Heating techniques could improve treatment of macular degeneration

Age-related macular degeneration is the primary cause of central vision loss and results in the center of the visual field being blurred or fully blacked out. Though treatable, some methods can be ineffective or cause unwanted side effects.
Jinglin Huang, a graduate student in medical engineering at Caltech, suggests inefficient fluid mixing of the injected medicine and the gel within the eye may be to blame. Huang will be discussing the effects of a thermally induced fluid mixing approach for AMD therapy during a session at the American Physical Society's Division of Fluid Dynamics 72nd Annual Meeting, which will take place on Nov. 23-26, 2019, at the Washington State Convention Center in Seattle.
The talk, "Thermal Effects on Fluid Mixing in the Eye," will be presented as part of the session on biological fluid dynamics: microfluidics.
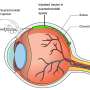
AMD usually starts as "dry" AMD, a disorder in which the macula—the central part of the retina, responsible for sending information about focused light to the brain to create a detailed picture—thins with age. Dry AMD is very common and is not treatable but may eventually evolve into "wet" AMD, which is more likely to result in vision loss. In wet AMD, abnormal blood vessels grow on the retina, leaking fluids under the macula. In the case of wet AMD, injections of medications called anti-vascular endothelial growth factor agents into the eye can help manage the disorder.
Huang said because the medication does not mix with the gel-like fluid in the eye—the vitreous—efficiently. Applying heat to the mixture can solve this problem.
"Because thermally induced mixing in the vitreous chamber can promote the formation of a circulation flow structure, this can potentially serve the drug delivery process," Huang said. "Since the half life of the drug is limited, this thermally induced mixing approach ensures that more drug of high potency can reach the target tissue."
To apply the thermally induced mixing technique, no changes in the injection procedure are needed. An additional heating step after the injection is all that is required.
"It can potentially reduce the amount of drug injected into the vitreous," said Huang. "It is definitely easy to be implemented."
Huang and her colleagues hope this work will inspire eye doctors to develop better treatment techniques and improve patient experiences.
More information: www.apsdfd2019.org/
Provided by American Physical Society