A fine-tuned microscopy technique offers breakthrough imaging of melanoma
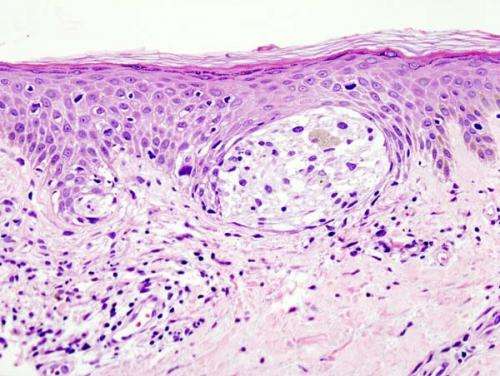
Melanoma is the deadliest form of skin cancer, with over 232,000 new cases and 55,000 deaths per year worldwide. Those with light-skin or red hair are often prone to hard-to-detect melanomas, often caused by properties of pigments within skin called melanins. People with fair skin have a higher concentration of the melanin known as pheomelanin in their skin, and a corresponding higher probability of developing melanoma—in particular, a difficult-to-detect subtype known as amelanotic melanoma. In high concentrations, pheomelanin is responsible for the orange-reddishness in hair, but is essentially invisible in skin.
While eumelanin, the brown-black pigment found in most melanomas, can be easily seen, the light colored pheomelanin is difficult to detect; even with advances in modern microscopy, understanding the pheomelanin molecule and its role in melanoma has eluded scientists.
Recently, researchers at Massachusetts General Hospital's Wellman Center for Photomedicine have made a breakthrough for spotting and studying this elusive molecule in skin. Sam Osseiran, a scientist on the team lead by Harvard University professor Conor Evans, will present their findings at the OSA Biophotonics Congress: Optics in the Life Sciences meeting, held 2-5 April in San Diego, California, USA.
The Evans group's research centers around the use of a high-resolution imaging technique called coherent anti-Stokes Raman Scatterings (CARS) microscopy, a variant of the more widely used Raman spectroscopy that enables chemically-specific imaging by means of detecting molecular vibrations.
Evans, whose translational research group specializes in microscopy and spectroscopy for understanding cancer and dermatology afflictions, says the common assumption about locating and imaging pheomelanin is that "there's really no good way to see this mostly invisible pigment when it occurs in skin."
But Massachusetts General's chief of dermatology, David Fischer, approached Evans and they decided to collaborate. Evans' research team took on the pheomelanin imaging challenge. "So my team put our heads together, scouring for ways to see it," Evans said.
While another optical technology, called transient absorption microscopy, does offer possibilities for studying pheomelanin, this method is complex and does not easily lend itself to clinical practice.
"We started to look through the Raman literature," Evans said. "Raman spectroscopy is a very mature technique that allows you to detect molecules by their unique chemical vibrations, which are themselves derived from the structure of the molecules. CARS microscopy is a coherent Raman tool that is akin to using a tuning fork to specifically detect molecular structures."
Fortunately, CARS microscopy proved successful for imaging pheomelanin. "Pheomelanin has a unique chemical structure, there is nothing else like it in the body," Evans said. "So, we started to look at the molecular structure and noticed there was a corresponding unique molecular vibration that might be useful for imaging the pigment with CARS microscopy."
Evans gives much of the credit to his research team, Sam Osseiran and post-doctoral researcher Tracy Wang, for leading the way in developing and refining the CARS microscopy method for imaging pheomelanin. In general, CARS microscopy utilizes two lasers focused on a sample whose energy difference is "tuned" to specific molecular vibrations to generate high resolution imaging information.
"The work led by Tracy was really rather novel application of CARS microscopy to target this biomolecule which no one else has tried to do before," Osseiran said. "We adjusted our system and aligned and tuned everything so that we could specifically target this one melanin pigment, pheomelanin."
Serendipitously, while developing their CARS imaging method, the group found a complementary method that could be used for the simultaneous detection of eumelanin called sum-frequency absorption (SFA) microscopy. SFA makes use of a signal modulation scheme that can detect both species of melanin. This additional imaging tool is important, as most humans produce both species within skin, making mapping the distribution and quantity of both pigments important.
"Sum-frequency absorption imaging allows you to visualize where all the melanin absorbers are within tissue," said Evans. "As both CARS and SFA can be carried out at the same time, these two techniques can be used together to simultaneously image both melanin pigments."
Wang and Osseiran believe their CARS and SFA method could be very helpful for future research on melanoma and its treatment, as well as observing the changes that occur with melanin species in different states. "We are adding another tool to our utility belt here in our investigations of melanoma," Osseiran said.
The study's original motivator, David Fischer, believes that a very important benefit of the work might be its potential role in diagnosing cancer.
"This may offer a brand-new tool for early diagnosis for some of the most lethal melanomas, possibly at a stage when they might still be curable," said Fisher. "Time and time again, it is proven that early diagnosis saves lives."
Provided by Optical Society of America