Scientists grow mouse eggs from stem cells in lab
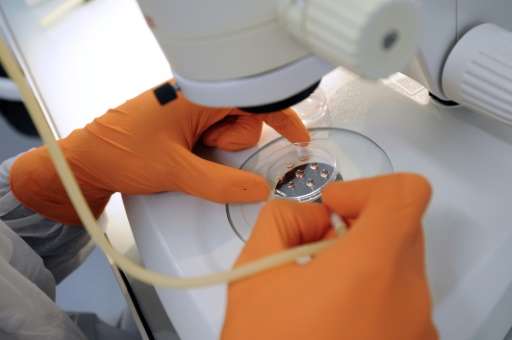
Japanese scientists said Monday they had grown mouse eggs entirely in the lab, then fertilised them to yield fertile offspring, a scientific first cautiously hailed by experts in human reproduction.
The technique—which involved coaxing stem cells into becoming mature eggs—was still much too risky and controversial to be reproduced in humans, commentators said.
"This is the first report of anyone being able to develop fully mature and fertilisable eggs in a laboratory setting right through from the earliest stages of oocyte (immature egg) development," commented Richard Anderson of the University of Edinburgh's MRC Centre for Reproductive Health.
While the technique may be useful to treat infertility "one day", the paper also showed "the complexity of the process and how it is a long way from being optimised," he said via the Science Media Centre in London.
Only a small number of embryos which grew from the eggs developed into normal mice.
The lab-grown eggs were more likely to have chromosomal abnormalities.
The authors of the paper—published in the science journal Nature—reported using two types of stem cell, which are neutral, juvenile cells that can become most any type of specialised cell of the body.
The first kind was harvested directly from mouse embryos, the team said, and the other created in the lab by reprogramming cells taken from mouse tail tips back into a juvenile state from which they can re-specialise.
The stem cells were grown into mature eggs, which were fertilised in the lab as well. The resulting embryos were then transferred into surrogate mice.
Of those that survived, both male and female pups were fertile and produced another generation of mice, the authors reported.
Ethical conundrum
"The data are primarily of interest to scientists, although potentially of clinical interest to those patients who lack eggs of their own," Martin Johnson, a professor of reproductive sciences at the University of Cambridge, wrote in a comment on the paper.
Congratulating the Japanese on a "remarkable achievement," he pointed out that there were, however, major limitations.
Not only was there a high risk of abnormalities, but the scientists had to add a type of cell, which can only be obtained from an embryo, to the petri dish during the egg maturation process.
This poses an ethical problem for human reproductive science.
One day these cells may also be grown in the lab, but this may take years, observers said.
Even if we could grow a human egg from stem cells, "the final and ultimate test for fully functional human 'eggs in a dish' would be the fertilisation using IVF, which is also ethically not allowed," said James Adjaye, director of the Institute for Stem Cell Research and Regenerative Medicine at Heinrich Heine University Duesseldorf.
Commentators said further study is needed into what happened to those mouse embryos that do not develop normally.
Earlier this year, scientists in Spain said they had created precursor sperm cells from human skin cells. And Chinese researchers in February said they had created mice from lab-grown sperm.
More information: Reconstitution in vitro of the entire cycle of the mouse female germ line, Nature (2016) DOI: 10.1038/nature20104
Journal information: Nature
© 2016 AFP