Multiple, co-existing groups of gut bacteria keep Clostridium difficile infections at bay
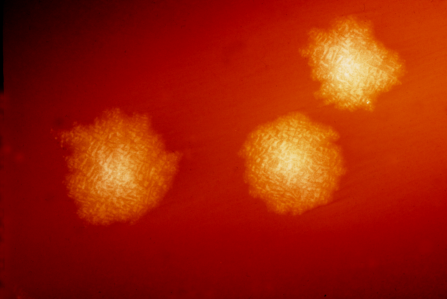
Multiple species of bacteria working together in healthy guts are responsible for keeping out nasty bacterial invader, Clostridium difficile, a hospital-acquired culprit responsible for 15,000 deaths each year. The study, published this week in mBio, the online open-access journal of the American Society for Microbiology, could lead to tests to predict which hospital patients are at highest risk of infection and better management of infections.
"Hospital-acquired C. difficile infections have bloomed as a problem in the last 10-15 years, representing $4.8 billion in added healthcare costs," says Patrick Schloss, a microbiologist at the University of Michigan in Ann Arbor who oversaw the study. "One of the biggest risk factors for someone acquiring C. difficile is exposure to antibiotics. That puts a huge pool of people at risk."
To mimic those patient conditions, Schloss's former graduate student, Alyxandria Schubert tested 8 antibiotics in 16 different treatment conditions to see how they altered the normal gut microbiota of mice. Then, she measured how those altered communities responded when exposed to C. difficile.
Not surprisingly, each treatment yielded different alterations in the communities, with different bacterial species increasing or decreasing in abundance. No single species accounted for either protection against or susceptibility to C. difficile.
"Mathematical modeling became really critical for the large amount of data we had," says Schloss. Previous work by the Schloss lab and others had hinted that protection against C. difficile colonization was likely due to multiple species within the gut microbiota. Ultimately, the team wanted to build a model that could use a mouse's starting gut bacterial community to predict that mouse's risk of infection.
To do that, the team applied a machine-learning algorithm to their entire dataset of the 16 treatment conditions and the resulting community-wide changes in bacterial species. In a sense, the algorithm acts akin to an email spam filter, says Schloss, using a 'forest' of decision trees to classify all the moving parts in a complicated data set.
The team built a mathematical model that could predict with about 90% accuracy whether a given mouse, starting with a particular gut bacterial community, would fall ill with C. difficile. The analysis also revealed the complex bacterial relationships that governed resistance to C. difficile.
Resistance was associated with members of the Porphyromonadaceae, Lachnospiraceae, Lactobacillus, Alistipes, and Turicibacter. Susceptibility to C. difficile, on the other hand, was associated with loss of these protective species and a rise in Escherichia or Streptococcus.
"Susceptibility is not all or nothing—it's extremely context dependent," says Schloss. He says that simply having a 'good' protective bacterial species present does not equal protection, nor does simply harboring one of the 'bad' bacterial species equal illness. "I think about it as a buffet, where you have to mix and match different ingredients to get resistance or sensitivity to C. difficile."
Having an accurate, predictive model in mice is a proof-of-principle that such a model could also work for human patients in a hospital setting. "If we could assess a patient's microbiota from a stool sample—especially if they are getting antibiotics—we could look at what bacteria are missing," says Schubert, now a postdoctoral researcher in the Schloss laboratory. "You could perhaps give patients a probiotic supplement with the goal of restoring their microbiota community structure to a healthy state."
Journal information: mBio
Provided by American Society for Microbiology