Computer simulator will improve radiation therapy for cancer patients
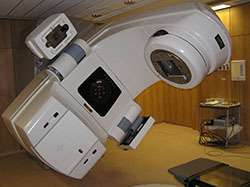
Using complex computational algorithms based on repeated sampling, a University of Arkansas graduate student helped spearhead a project to develop a computer simulator that provides customized electron beam tunings for radiation therapy. The research will help cancer centers provide better radiation therapy.
Justin LeBlanc, a Distinguished Doctoral Fellow and doctoral candidate in economics in the Sam M. Walton College of Business, and colleagues developed and verified the simulator and a design process as part of his master's thesis in physics at Louisiana State University. The study has been published in the Journal of Applied Clinical Medical Physics.
In radiation therapy, linear accelerators deliver highly focused beams of electrons to destroy cancerous cells. The accelerator produces a small, intensely concentrated beam of electrons called a pencil beam. For this to be useful clinically it must be broadened to cover the patient's tumor. Dual-scattering systems are designed for this purpose. They help ensure the electrons deposit their energy into the patient's cancerous tissue while sparing surrounding, healthy tissue.
The current approach for designing dual-scattering systems is a conventional, one-size-fits-all standard, because their design proposes a nearly infinite number of solutions for achieving any one facility's desired specifications.
"Until now, the design process had never been done analytically," LeBlanc said.
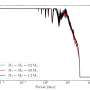
The simulator facilitates better design of dual-scattering foil systems. When the geometry of such a system is specified, the simulator allows the user to vary primary and secondary scattering foil material and thickness and to see results in approximately 100 milliseconds, about 10 million times faster than Monte Carlo simulations, which are simulations and computational algorithms that rely on random sampling to obtain results for extremely complex problems that have only numerical solutions.
The rapid design capability allows an initial optimization to be obtained, which can then be refined and verified with subsequent Monte Carlo calculations and measurements. This process can be used to facilitate a better design of dual-scattering foil systems for improved patient treatment.
"The user user-friendly interface and real-time nature of the simulator also make it an effective educational tool for gaining a better understanding of the effects that various system parameters have on dose profiles," LeBlanc said. "In other words, it will help medical physicists and linear accelerator designers to better understand the physics behind the equipment with which they will be working."
Provided by University of Arkansas