Tiny inhaled particles take easy route from nose to brain
In a continuing effort to find out if the tiniest airborne particles pose a health risk, University of Rochester Medical Center scientists showed that when rats breathe in nano-sized materials they follow a rapid and efficient pathway from the nasal cavity to several regions of the brain, according to a study in the August issue of Environmental Health Perspectives.
Researchers also saw changes in gene expression that could signal inflammation and a cellular stress response, but they do not know yet if a buildup of ultrafine particles causes brain damage, said lead author Alison Elder, Ph.D., research assistant professor of Environmental Medicine.
The study tested manganese oxide ultrafine particles at a concentration typically inhaled by factory welders. The manganese oxide particles were the same size as manufactured nanoparticles, which are controversial and being diligently investigated because they are the key ingredient in a growing industry -- despite concerns about their safety.
Nanotechnology is a new wave of science that deals with particles engineered from many materials such as carbon, zinc and gold, which are less than 100 nanometers in diameter. The manipulation of these materials into bundles or rods helps in the manufacturing of smaller-than-ever electronics, optical and medical equipment. The sub-microscopic particles are also used in consumer products such as toothpaste, lotions and some sunscreens.
Some doctors and scientists are concerned about what happens at the cellular level after exposure to the ultrafine or nano-sized particles, and the University of Rochester is at the forefront of this type of environmental health research. In 2004 the Defense Department selected the University Medical Center to lead a five-year, $5.5 million investigation into whether the chemical characteristics of nanoparticles determine how they will interact with or cause harm to animal and human cells.
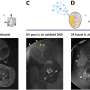
In the current study, the particles passed quickly through the rats' nostrils to the olfactory bulb, a region of the brain near the nasal cavity. They settled in the striatum, frontal cortex, cerebellum, and lungs.
After 12 days, the concentration of ultrafine particles in the olfactory bulb rose 3.5-fold and doubled in the lungs, the study found. Although the ultra-tiny particles did not cause obvious lung inflammation, several biomarkers of inflammation and stress response, such as tumor necrosis factor and macrophage inflammatory protein, increased significantly in the brain, according to gene and protein analyses.
"We suggest that despite differences between human and rodent olfactory systems, this pathway is likely to be operative in humans," the authors conclude.
Source: University of Rochester Medical Center