Stopping Candida in its tracks
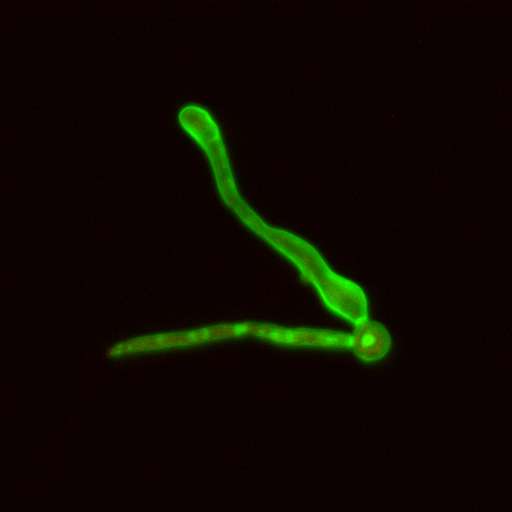
Scientists are one step closer to understanding how a normally harmless fungus changes to become a deadly infectious agent.
The opportunistic fungus Candida albicans is normally a harmless member of the microbial community that occupies the human gut. However, it is also the causative agent of oral thrush and, more severely, it is responsible for approximately 400,000 life-threatening blood infections each year. Understanding what triggers this switch from benign resident to dangerous enemy could help to protect those who are most at risk—including the elderly, HIV patients and those receiving organ transplants.
Most of the time, the human immune system is able to suppress C. albicans so that it lives in a harmless, round "yeast" form. When the immune system is compromised however—such as during organ transplants to prevent tissue rejection—the fungus switches to a new and deadly mode of growth. The round cells start to produce long filaments (called hyphae) which burrow into the underlying tissue layers. This allows the fungus to invade and form infectious colonies.
Researchers at the University of Aberdeen have recently found that a small signalling molecule, called Rsr1, controls the steering mechanisms that hyphae use to probe host surfaces. "Rsr1 helps the hyphae to penetrate tissues and to steer through barriers" says Tina Bedekovic, who studies this protein as part of her research. "Without Rsr1, the ability of the fungus to cause disease is significantly reduced". Brewer's Yeast (Saccharomyces cerevisiae) does not form filaments but Rsr1 still functions to control polarised growth. In this case, it is known to be activated by another molecule called Bud5. When the researchers deleted Bud5 in C. albicans, however, its hyphae were still able to penetrate tissues and steer around obstacles. This suggests that Rsr1 in C. albicans is regulated by a different activator specific for this function.
According to Tina Bedekovic, identifying this activator may help to develop clinical treatments. "Humans also have a version of Rsr1 and Bud5 so it is unlikely that we could develop a drug to inhibit these in C. albicans without also affecting human cells" she says. "But if they are part of a fungus-specific signalling pathway that controls directional growth, this could be targeted with therapeutic drugs without harming the patient".
The researchers now plan to investigate which molecules can bind to Rsr1 in C. albicans and, from these, to identify the activator required for invasive filamentous growth.
More information: This work is being presented at the Annual Meeting of The Society for Experimental Biology, Prague on Friday 3rd July.
Provided by Society for Experimental Biology


















