Retinal rescue: Cells derived from human embryonic stem cells reverse retinal degeneration
A new study reports that transplanted pigment-containing visual cells derived from human embryonic stem cells (hESCs) successfully preserved structure and function of the specialized light-sensitive lining of the eye (known as the retina) in an animal model of retinal degeneration. The findings, published by Cell Press in the October 2nd issue of the journal Cell Stem Cell, represent an exciting step towards the future use of cell replacement therapies to treat devastating degenerative eye diseases that cause millions of people worldwide to lose their sight.
The retinal pigment epithelium (RPE) is a layer of pigmented cells sandwiched between the visual retinal cells, called photoreceptors, and the nourishing blood vessels at the back of the eye. The RPE provides essential support to the retinal photoreceptors and is critical for normal vision. Deterioration of the RPE plays a central role in the progression of diseases such as age-related macular degeneration and sub-types of retinitis pigmentosa. These conditions are associated with a progressive loss of vision that often leads to blindness.
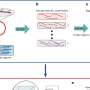
"Although there are a variety of therapeutic approaches under development to delay the degenerative process, the grim reality is that many patients eventually lose their sight," explains Dr. Benjamin Reubinoff, a senior author of the study. "Cell therapy to replenish the degenerating RPE cells may potentially halt disease progression." Dr. Reubinoff and Dr. Eyal Banin who led the study, with their colleagues from Hadassah-Hebrew University Medical Center in Jerusalem, developed conditions to guide hESCs to differentiate into functional RPE-like cells in the laboratory.
The researchers found that nicotinamide (vitamin B3, NIC) and Activin A, an important growth factor, promoted differentiation of hESCs towards an RPE fate. The hESC-derived RPE-like cells, which could be identified by their characteristic black pigment, exhibited multiple biological properties and genetic markers that define authentic RPE cells. Further, the cells successfully delayed deterioration of retinal structure and function when they were transplanted into an animal model of retinal degeneration caused by RPE dysfunction.
Taken together, the results demonstrate that NIC and Activin A promoted the differentiation of hESCs towards an RPE fate. The hESC-derived cells exhibited the defining characteristics associated with RPE and successfully rescued the retina when transplanted into an animal model of retinal degeneration. "Our findings are an important step towards the potential future use of hESCs to replenish RPE in blinding diseases," concludes Dr. Banin.
Source: Cell Press (news : web)