Breakthrough in fight against Hendra virus
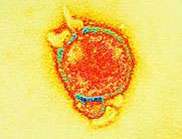
(PhysOrg.com) -- There has been a breakthrough in the fight against the deadly Hendra virus following the development of a treatment which shows great potential to save the lives of people who become infected with the virus.
A scientific team from CSIRO and the US has demonstrated that administering human monoclonal antibodies after exposure to Nipah virus, which is closely related to Hendra virus, protected animals from challenge in a disease model.
According to CSIRO's Dr Deborah Middleton, who led the experiments at Australia's maximum biosecurity facility, CSIRO's Australian Animal Health Laboratory (AAHL) in Geelong, said the findings are extremely encouraging.
"Our research clearly suggests that an effective treatment for Hendra virus infections in humans should be possible, given the very strong cross-reactive activity this antibody has against Hendra virus," she said.
Antibodies - proteins found in blood or other bodily fluids of vertebrates - are used by the immune system to identify and neutralise bacteria and viruses.
First identified in Brisbane and isolated by CSIRO scientists in 1994, Hendra virus, which spreads from flying foxes, has regularly infected horses in Australia. Of the 12 equine outbreaks, four have led to human infection, with four of the seven known human cases being fatal, the most recent of these in September 2009. Human infection results from close contact with the blood and/or mucus of infected horses.
Dr Middleton said the success of the antibody will probably depend on dose and time of administration.
"As Hendra and Nipah viruses cause severe disease in humans, a successful application of this antibody as a post-exposure therapy will likely require early intervention.
"To make clinical use of it against these viruses, it will need to be prepared under proper manufacturing guidelines, carefully evaluated again in animal models and safety tested for human use. We hope this demonstration of antiviral activity will lead to some immediate activities to facilitate further development for its use in humans," Dr Middleton said.
The results of this latest research, conducted in collaboration with scientists from the US's Uniformed Services University of the Health Sciences, National Cancer Institute and the National Institutes of Health in the US, were published today in the journal PLoS Pathogens.
More information: dx.plos.org/10.1371/journal.ppat.1000642
Provided by CSIRO (news : web)