A novel target for therapeutics against Staph infection
Researchers at the Texas A&M Health Science Center Institute of Biosciences and Technology, and the University of Edinburgh have uncovered how a bacterial pathogen interacts with the blood coagulation protein fibrinogen to cause methicillin-resistant Staphylococcus aureus (MRSA) infections, a finding that could aid in developing therapeutics against the potentially deadly disease. Their work appears November 28 in the open-access journal PLoS Pathogens.
Once occurring more commonly in healthcare facilities, but now affecting segments of the general population, MRSA is a bacterial pathogen responsible for a range of diseases from mild skin infection to life-threatening sepsis. Even with antibiotics, these infections can still be fatal.
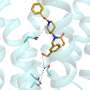
Senior author Magnus Höök, Ph.D. and his colleagues carried out biochemical and structural studies to determine the binding mechanism of clumping factor A (ClfA), a surface protein that plays an important role in the pathogenesis of S. aureus. The group found that ClfA binds to the blood-clotting protein fibrinogen (Fg) at a site that is also responsible for inducing platelet activation and thrombosis (clot inside a blood vessel).
The results show significant structural differences in how staphylococcal and platelet receptor proteins recognize fibrinogen. By exploiting this difference in recognition, the researchers show that agents could be designed that inhibit the ClfA–Fg interaction but do not interfere with the interaction of Fg with the platelet integrin, therefore avoiding unwanted side effects on the circulatory system.
Citation: Ganesh VK, Rivera JJ, Smeds E, Ko Y-P, Bowden MG, et al. (2008) A Structural Model of the Staphylococcus aureus ClfA–Fibrinogen Interaction Opens New Avenues for the Design of Anti-Staphylococcal Therapeutics. PLoS Pathog 4(11): e1000226. doi:10.1371/journal.ppat.1000226
dx.plos.org/10.1371/journal.ppat.1000226
Source: Public Library of Science