Preclinical Tests Show Acid-Sensitive Nanoparticles Treat Ovarian Cancers with Little Toxicity
Last year, members of the Alliance for Nanotechnology in Cancer based at Northeastern University and the Massachusetts Institute of Technology demonstrated that acid-sensitive polymer nanoparticles could boost the delivery of anticancer drugs into the acidic interior of tumors.
Now, that same group of investigators has shown that these nanoparticles are effective at suppressing tumor growth when tested in an animal model of human ovarian cancer. In addition, animals treated with this nanoparticle formulation do not appear to experience adverse side effects that often limit the ability of patients to tolerate chemotherapy. The researchers reported the results of their preclinical work in the journal Cancer Chemotherapy and Pharmacology.
Mansoor Amiji, Ph.D., of Northeastern University, and Robert Langer, Ph.D., at MIT, led the team of investigators that tested the ability of biodegradable, pH-sensitive nanoparticles to safely and effectively deliver paclitaxel to rapidly growing tumors.
These nanoparticles are made of several polymers, each of which contributes useful characteristics to the nanoparticle, such as water-solubility, water-insoluble drug packaging, and ability to repel proteins in blood and avoid elimination by immune system cells. The nanoparticles are stable in blood and normal tissues, but fall apart under the acidic, or low pH conditions, characteristic of virtually all solid tumors.
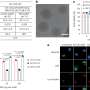
To test the utility and safety of these polymer nanoparticles, the researchers loaded them with anticancer agent paclitaxel and administered them to mice with human ovarian tumors. The researchers assessed therapeutic efficacy by measuring the volume of the tumors over the course of four weeks after receiving a single dose of either the paclitaxel-loaded nanoparticle or paclitaxel alone. After four weeks, tumors in the mice treated with the nanoparticle formulation were about half the size of those treated with paclitaxel alone. In addition, tumors removed from the animals treated with the nanoparticle formulation weighed 80 percent less than those treated with paclitaxel alone.
The investigators also measured changes in the animals’ weight and blood cell counts over the course of the four-week experiment. These data indicated that neither the nanoparticle formulation nor paclitaxel alone triggered therapy-limiting side effects after a single dose of drug.
This work, which was supported by the National Cancer Institute, is detailed in a paper titled, “Poly(ethylene oxide)-modified poly(beta-amino ester) nanoparticles as a pH-sensitive system for tumor-targeted delivery of hydrophobic drugs: part 3. Therapeutic efficacy and safety studies in ovarian cancer xenograft model.” This paper has been published online in advance of print publication. An abstract of this paper is available through PubMed.
Source: National Cancer Institute