Inflammation triggers cell fusions that could protect neurons
Chronic inflammation triggers bone marrow-derived blood cells to travel to the brain and fuse with a certain type of neuron up to 100 times more frequently than previously believed, according to a new study from the Stanford University School of Medicine.
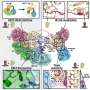
After the fusion, the blood-cell nuclei begin to express previously silent, neuron-specific genes. The surprise finding in mice suggests that the creation of the fused cells, called heterokaryons, may possibly play a role in protecting neurons against damage and may open new doors to cell-mediated gene therapy.
"This finding was totally unprecedented and unexpected," said senior author Helen Blau, PhD, the Donald E. and Delia B. Baxter Professor and director of the Baxter Laboratory in Genetic Pharmacology. "We're getting hints that this might be biologically important, but we still have a lot to learn." The research, led by Clas Johansson, PhD, a postdoctoral scholar in Blau's laboratory, will be published online in Nature Cell Biology on April 20.
The bone marrow-derived cells are known as blood stem cells, or hematopoietic stem cells. They can give rise to all the blood and immune cells in the body. Although the progeny of these hematopoietic stem cells have previously been shown to fuse with a variety of other cell types in the body, this fusion occurs so infrequently that it had been thought to have little biological significance.
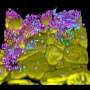
Purkinje neurons are large cells in a portion of the brain known as the cerebellum, which is involved in balance and motor control. They form junctions between many other neurons, and they do not regenerate. They are the only cell in the brain shown by Blau and others to fuse with these bone marrow-derived cells in mice and humans.
Previous studies investigating this cell fusion in mice relied on the use of lethal doses of radiation to abolish one mouse's hematopoietic system prior to introducing blood stem cells engineered to express a green fluorescent protein. The new blood stem cells would then entirely repopulate the animal's now-absent hematopoietic system with green-fluorescing cells whose origin could be easily identified. The researchers could then pick out heterokaryons in the brain by looking for green neurons against a neutral background.
The researchers, in collaboration with scientists at the University of British Columbia in Vancouver, used this technique in the current study to transplant a single hematopoietic stem cell and prove that the heterokaryons in the brain were derived from blood. However, because such high doses of radiation are known to break down the natural barrier that restricts the flow of cells and molecules between the brain and the blood, Blau and her colleagues wondered if this fusion would still occur under less physiologically traumatic conditions.
They used a technique called parabiosis to introduce blood cells expressing green fluorescent protein into an unmodified animal. In parabiosis, two mice are surgically joined in such a way that they share a circulatory system. One mouse had been engineered to express the green protein in all its cells, and one had not. Because the animals shared a blood supply for several weeks, about half of the blood cells in the unmodified mouse expressed the green protein-enough to enable the researchers to detect fused cells in the brain.
The researchers found evidence of fusion between blood cells and Purkinje neurons in this radiation-free system 20 to 26 weeks after surgery. In fact, green heterokaryons were identifiable for up to 20 weeks after the mice were separated, when most of the blood cells in the unmodified mouse had been regenerated as non-colored cells.
But then Johansson saw something surprising. As in previous experiments, most of the mice had very low numbers of fused cells in their cerebellums, but a few had more. Up to 100 times more.
"Clas noted significantly more heterokaryons than we ever had in the past," said Blau, "from fewer than 10 in an entire animal to several hundred." When the researchers looked more closely, they found that those animals with higher-than-expected numbers of fused cells also had an inflammatory skin condition common to aging laboratory mice called idiopathic ulcerative dermatitis. This type of chronic inflammation affects the entire immune system of the animal and causes a systemwide immune response.
The researchers confirmed that the remarkable increase in the numbers of fused cells was related to inflammation by using the traditional radiation/bone marrow transplant approach in mice with dermatitis. Finally, they counted the fused cells that formed in a mouse model of multiple sclerosis - an autoimmune disease characterized by inflammation and damage of the central nervous system. Neurologist and multiple sclerosis specialist Lawrence Steinman, MD, professor of neurology and neurological sciences at the medical school, co-authored the research and provided the mouse model for study. Heterokaryons in some of these mice numbered in the thousands.
Even more intriguing than the inflammation-induced increase in numbers was a cross-species experiment that showed nuclei from rat blood stem cells that had fused to Purkinje cells in mice stop expressing blood cell proteins and begin to express rat neuron-specific gene products. This switch exemplifies a type of genetic reprogramming that has been a source of ongoing debate and great interest in the world of stem cell research. Such reprogramming is critical to the regeneration of functional tissues by stem cells.
"What we're seeing is that this phenomenon is happening in real life," said Blau, who next plans to study whether such fusions can rescue damaged or dying Purkinje neurons. "We don't know yet if this function is beneficial, but we now know that there are sites where it happens at fairly high frequencies under certain conditions, and that these nuclei can even be reprogrammed."
Source: Stanford University