Worms produce surprise insight into human fever
Give or take a few dozen trillions, a human adult has about 70 trillion cells. An adult Caenorhabditis elegans roundworm has exactly 959 cells.
Yet we have an awful lot in common, says Alejandro Aballay of Duke University, who has been exploring two “highly conserved” cell-signaling pathways for innate immunity shared by worms and humans. For one, we have a lot of common enemies, particularly soil-borne pathogens. C. elegans, of course, lives in the soil. Human populations merely ingest soil by the ton in our food, on our hands, and suspended in our drinking water.
Some of these basic pathways that set off the worm’s innate immune defenses have homologs—similar proteins in mammal cells, including ours. These conserved pathways are involved in many similar “effector” strategies against hostile bugs peristalsis, low gut pH, lytic enzymes, and antimicrobial peptides to prevent microbial colonization of the intestine.
In dissecting two conserved pathways required for C. elegans immunity to bacteria, Aballay found a wealth of data on innate immunity plus a surprising insight into another classic metazoan response to
infection fever.
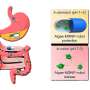
The first pathway was p38 MAPK/CED-3, which is also required for the activation of programmed cell death under certain stresses. The other was a heat shock transcription factor-1 (HSF-1) pathway, which is elicited by increased temperature independently of p38 MAPK/CED-3. Aballay identified genes in both pathways that encoded immunity effector molecules plus relevant signaling molecules and transcription factors. In fluorescently labeled transgenic worms, he mapped gene expression in the two target pathways as they came into direct contact with a small zoo of pathogenic microbes.
The big surprise was the discovery that the HSF-1 pathway was required for C. elegans immunity against Pseudomonas aeruginosa, Salmonella enterica, Yersinia pestis, and Enterococcus faecalis. It indicated that HSF-1 is part of a broad, multi-pathogen defense pathway. And it also suggested something new about fever, says Aballay.
Fever is an ancient immune mechanism used by metazoans in response to microbial infections. Warm-blooded “homeotherms” like rats (and people) can increase their internal body temperature in response to infection, yet even cold-blooded “poikilotherms” like worms migrate toward warmer environments in response to infections. But the mechanism of fever as a response to infection is still largely unknown. The activation of the HSF-1 pathways by heat shock and its function in C. elegans
immunity provides both a molecular explanation for the beneficial role of behavioral fevers in poikilotherms and a mechanism by which fever works in metazoans, says Aballay.
It also raises questions about the HSF-1 pathway in humans and whether drugs currently used to reduce fever in infected patients may make matters worse by preventing activation of the HSF-1 pathway. Aspirin and similar anti-inflammatory drugs, which reduce fever but also activate
HSF-1 signaling, could offer the best of both worlds, says Aballay. He also points out that new drugs designed to activate HSF-1 are already in clinical trials for treating neurodegenerative diseases. “Our work opens the possibility of using co-inducers of HSF-1 to boost immunity to
treat infectious diseases and immunodeficiencies,” says Aballay.
Source: American Society for Cell Biology