Human stem cells can contribute to a developing mouse embryo, despite evolutionary differences
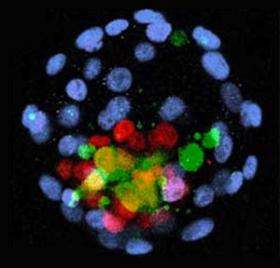
Using a newly derived line of human embryonic stem cells, Rockefeller University researchers have coaxed human cells to grow in mouse tissue.
Ali Brivanlou, an embryologist who specializes in studying how the nervous system develops, and his colleagues demonstrated that despite the evolutionary distance and difference in gestational time, a small number of human embryonic stem cells can contribute to the formation of derivatives of all three germ layers of a developing mouse embryo. The result, reported as the cover story of the July 1 issue of the journal Developmental Biology, is a groundbreaking means of both elucidating the beginning of human embryonic development and serving as the starting point from which to understand their potential therapeutic secrets of human embryonic stem cells.
Thanks to Brivanlou and colleagues Daylon James, Scott Noggle and Tomasz Swigut, the research community has a new template for studying the early decisions that an embryo makes as it develops into various body tissues.
“At the beginning of the 21st century, it is embarrassing that we know more about how a worm, fly, frog, bird or mouse develops than we do about ourselves. Although we have the human genome in our pockets, we remain ignorant about our own development,” says Brivanlou, professor and head of the Laboratory of Molecular Vertebrate Embryology at Rockefeller. “Studying human embryonic stem cells in a mouse embryo distinguishes what the cells actually do in an in vivo environment, versus what they can do in a Petri dish.”
Embryonic stem cells offer a window into human embryology. However, for obvious reasons, scientists cannot study cell fate in developing human embryos. The next best model for these studies is to be able to observe the behavior of embryonic cells in the context of an actual embryo. Brivanlou and colleagues watched the human cells in the context of mouse embryos. The choice of merging human and mouse embryonic cells makes scientific sense as the molecular and cellular aspects of mouse development has been the subject of intense scrutiny for the past few decades. Thus, the mouse embryo presents a platform in which the molecular basis of human embryonic differentiation can be quantitatively tested.
“Ali Brivanlou and his colleagues have performed a series of elegant, technically difficult experiments,” says Paul Nurse, president of The Rockefeller University. “Their findings provide the first hard evidence of how human stem cells perform in an embryonic environment, research that is crucial before their clinical application can be considered.”
Dubbed “RUES1” (Rockefeller University Embryonic Stem Cell Line 1), the new human embryonic stem cell line was derived using private funds provided by the Juvenile Diabetes Research Foundation. The researchers, using private funds provided by Rockefeller University, then combined mouse and human embryonic cells in a series of experiments designed to test whether human embryonic stem cells could thrive in a mouse embryo. If the RUES1 cells survived, they could be evaluated as functioning stem cells, namely cells with both the power to self-renew and to form all tissue types. The experiments were guided by recommendations from Rockefeller University’s Human Embryonic Stem Cell Bioethics Committee and are within the guidelines for human embryonic stem cell research set forth in April 2005 by the U.S. National Academy of Sciences.
Using three-day-old mouse embryos, the research team injected 10 to 15 human embryonic stem cells per embryo and studied them first in vitro for six days. About 15 percent of these hybridized embryos developed with RUES1 cells coexisting with those of the mouse.
Interestingly, the Rockefeller team found that RUES1 cells not only integrate into the mouse embryo when put in close contact, but actually migrate to the inner cell mass, the very same region in which they were originally located in the human embryo. In other words, the human embryonic stem cells moved to the correct address in their strange new environment. That these two cell types can develop together is an exciting result, given that these two species are separated by an evolutionary distance of 100 million years. RUES1 cells divided and differentiated alongside their mouse counterparts, suggesting the possibility that the speed of differentiation of human cells can be reprogrammed to the faster speed of the mouse.
After another day, when the mouse embryos began forming the first types of identifiable tissue known as the three germ layers — ectoderm, mesoderm and endoderm — RUES1 cells could be found in all three types. After a total of six days, RUES1 contribution was clearly evident.
Brivanlou’s team pursued its observations by returning the hybridized three-day mouse embryos to the womb of a pregnant mouse. This in vivo experiment permitted the researchers to study the developmental potential of what happens to RUES1 cells in mouse embryos. Although most of the embryos encountered problems staying on course, one hybridized mouse embryo developed normally. In this embryo, which was halted on day nine of development, 10 RUES1 cells were found — integrated into each of the three germ layers. This result indicates that RUES1 cells are capable of contributing to a developing mouse embryo. Until now, says Brivanlou, no other research team has reported this unexpected compatibility of such early embryonic human and mouse cells.
“We have shown that despite separation by 100 million years of evolution, human and mouse embryonic cells still share basic mechanisms of differentiation,” Brivanlou says. “This is the first step in a very long journey to both a basic understanding of human development and to the clinical use of human embryonic stem cells.”
Source: Rockefeller University