Discovery of key malaria proteins could mean sticky end for parasite
Scientists funded by the Wellcome Trust have identified a key mechanism that enables malaria-infected red blood cells to stick to the walls of blood vessels and avoid being destroyed by the body's immune system. The research, published today in the journal Cell, highlights an important potential new target for anti-malarial drugs.
Malaria is one of the world's biggest killers, killing over a million people every year, mainly children and pregnant women in Africa and south east Asia. It is caused by the malaria parasite, which is injected into the bloodstream from the salivary glands of infected mosquitoes. There are a number of different species of parasite, but the deadliest is the Plasmodium falciparum parasite, which accounts for 90% of deaths from malaria.
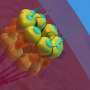
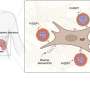
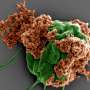
The malaria parasite infects healthy red blood cells, where it reproduces, producing up to thirty-two new daughter parasites. The parasite secretes a "glue", known as PfEMP1, which travels to the surface of the infected red blood cells, leading to the formation of the knobs on the surface of the cells. The cells become sticky and adhere to the walls of the blood vessels. This prevents the cells being flushed through the spleen, where the parasites would be destroyed by the body's immune system, but also restricts blood supply to vital organs.
Now, an international collaboration of scientists has identified eight new proteins that transport the P. falciparum parasite's "glue" to the surface of the infected red blood cells. The researchers, led by Professor Alan Cowman from the Walter and Eliza Hall Institute of Medical Research in Melbourne, Australia, have shown that removing just one of these proteins prevents the infected red blood cells from sticking to the walls of the blood vessels.
"These findings greatly enhance our understanding of how the malaria parasite commandeers the red blood cell for its own survival and avoids our immune defences," says Professor Cowman. "They also suggest that a drug that targets the 'stickiness' proteins could be an effective treatment for malaria."
Malaria is currently treated using drugs that kill the parasites. However, as the parasites evolve, they have become increasingly resistant to existing treatments such as chloroquine and mefloquine, and there is some evidence of increasing resistance against even the most effect and newest treatments, artemisinin derivatives such as artesunate.
"Malaria parasites are evolving, making our current treatments increasingly less effective," says Professor Alister Craig from the Liverpool School of Tropical Medicine, who collaborated on the project. "This suggests we need to approach the problem using a different strategy. A drug which prevents disease rather than killing the parasite might be important because it could retain natural inoculation in the patient, limiting damage caused by the parasite and providing protection from further infection."
The research was carried out by interfering with the function of specific genes on a scale not previously attempted in the malaria parasite. By blocking or "knocking out" the function of these genes the team was able to identify those important for allowing the parasite to stick to the walls of blood vessels.
Source: Wellcome Trust