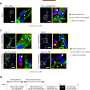
Researchers uncover process behind heart muscle contraction
Researchers from the University of Pittsburgh and the University of Chicago were able to control heart muscle function in a new way after discovering the previously unknown role of two enzymes in heart muscle contraction, as detailed in the April 11 cover story of the Journal of Biological Chemistry.
Although in the early stages, the research provides fresh knowledge of how heart muscle functions and also holds early potential as a treatment for various heart diseases—including congestive heart failure—that is possibly less taxing on the heart than current regimens.
Experiments on slivers of heart muscle revealed that heart muscle contractions can be regulated by the enzymes histone acetyltransferases (HATs) and histone deacetylases (HDACs), explained Pitt professor Sanjeev Shroff, the Gerald McGinnis Chair of Bioengineering in the Swanson School of Engineering. Shroff and Pitt research associate Stephen Smith collaborated with Mahesh Gupta, an associate professor of surgery at the University of Chicago, and his research associate Sadhana Samant. The project was funded by a grant from the National Institutes of Health.
The team found that HATs and HDACs influence acetylation of certain heart muscle proteins, a process wherein a radical cluster of atoms called an acetyl group attach to a protein and change its function. HATs facilitate acetylation, and HDACs remove the acetyl group. The team discovered that acetylation renders the muscle fiber more sensitive to calcium, which causes the muscle to contract.
“This is a completely new process in the area of heart muscle contraction,” Shroff said. “Acetylation is widely known to regulate such events inside the cell nucleus as gene regulation, but it’s never before been associated with heart muscle contraction.”
Furthermore, Shroff and his colleagues could intervene in this microscopic process to control heart muscle contraction. By inhibiting HDACs, they increased the calcium sensitivity of the muscle fibers and strengthened contraction.
As a possible treatment for such conditions as congestive heart failure, this technique could present an alternative to current therapies that counteract heart muscle weakness by boosting cellular calcium content, Shroff said. The heightened calcium improves muscle contraction but also results in more energy consumption in hearts that often are energy-starved to begin with.
In contrast, inhibiting HDAC alters a natural process to make heart muscle more sensitive to the prevailing level of calcium, he said.
“We did not create this process—we are just manipulating what is already there,” Shroff explained. “The physiology to block HDAC is already there, and we just took advantage of that. This perturbation does not require greater mobilization of calcium, so we won’t end up with increased cardiac energy consumption. That’s been the Achilles heel of treatment so far.”
The team’s next step involves examining HAT- and HDAC-driven regulation of cardiac contraction in the whole animal rather than just muscle samples. Then it can better determine the overall significance of the newly discovered process to the intact heart function and its therapeutic potential.
“We want to see how much protein acetylation matters when operating alongside all the other processes in the heart and the body,” Shroff said. “If this process is shown to be significant under these conditions, it will be an exciting finding.”
Source: University of Pittsburgh