Cellular Pathway Yields Potential New Weapon in Vaccine Arsenal
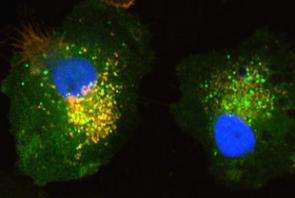
When a cell has to destroy any of its organelles or protein aggregates, it envelops them in a membrane, forming an autophagosome, and then moves them to another compartment, the lysosome, for digestion.
Two years ago, Rockefeller University assistant professor Christian Münz showed that this process, called autophagy, sensitizes cells for recognition by the immune system’s helper T cells. But he didn’t know how often this pathway is used or how efficient it is. Now, a new study published online today in the journal Immunity goes a long way toward addressing these questions and shows that the pathway is so common that it could be a valuable new way of boosting vaccine efficacy.
There are two types of T cells: Helper T cells encourage their counterpart, killer T cells, to hunt down and attack invading pathogens. T cells typically recognize antigens only once they’re presented to them by major histocompatibility compex (MHC) scaffolding molecules on a cell’s surface. Antigens on MHC class I molecules are recognized by killer T cells and had originally been thought to come only from sources inside a cell (proteins from the nucleus or other cellular part); those on MHC class II molecules are recognized by helper T cells and had been thought to come from sources outside the cell, such as fragments of dead, infected cells. But as Münz discovered two years ago, an autophagy pathway allows intracellular antigens to be presented on MHC class II molecules.
Now Münz, head of Rockefeller’s Laboratory of Viral Immunobiology, and Dorothee Schmid, a graduate student in the lab, have shown that the autophagy pathway is far more widespread than they thought: They found that a surprising number of cells with MHC class II molecules on their surfaces used the autophagy pathway. In skin (epithelial) cells and two other types of immune cells (dendritic and B cells), 50 to 80 percent of the autophagosomes moved into the loading compartment for MHC class II molecules. “For types of cells that upregulate MHC class II upon inflammation -- epithelial cells of infected organs, for instance -- one could assume that they might actually use the autophagy pathway fairly frequently,” Münz says.
Then, to test the pathway’s effectiveness, the researchers targeted an influenza antigen directly to autophagosomes. They found that they were able to increase antigen presentation by MHC class II molecules, subsequently boosting helper T cell recognition of viral antigens. “This targeting pathway could be very efficient for vaccine development,” Münz says, especially for recombinant viral vaccines like those against HIV. “Killer T cell responses are usually short-lived. But if you can increase recognition by helper T cells, then you’ll be more likely to maintain the killer T cell response and establish immunological memory.”
Source: Rockefeller University