Natural protein stops deadly human brain cancer in mice
Scientists from Johns Hopkins and from the University of Milan have effectively proven that they can inhibit lethal human brain cancers in mice using a protein that selectively induces positive changes in the activity of cells that behave like cancer stem cells. The report is published this week in Nature.
The most common type of brain cancer-glioblastoma-is marked by the presence of these stem-cell-like brain cells, which, instead of triggering the replacement of damaged cells, form cancer tissue. Stem cells, unlike all other cells in the body, are capable of forming almost any kind of cell when the right "signals" trigger their development.
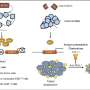
For their treatment experiment, the researchers relied on a class of proteins, bone morphogenic proteins, that cause neural stem-cell-like clusters to lose their stem cell properties, which in turn stops their ability to divide.
First they pretreated human glioblastoma cells with bone morphogenic protein 4 (BMP4), then injected these treated cells into mouse brains. In mice injected with cells that were not pretreated, large, invasive cancers grew. In the mice with BMP4-treated cells, no cancers grew at all. Three to four months after injection, all mice that got untreated cells died, and nearly all mice with BMP4-treated cells were alive.
Next, the scientists delivered slow-release BMP4-containing "beads" directly into mouse brains with implanted glioblastoma cells. Mice that got empty beads developed large malignant tumors and died. Mice with BMP4 beads survived much longer, and 80 percent survived four months after cancer cell implants.
"Our idea is to treat patients with BMP4 or something like it right after surgery to remove glioblastoma in hopes of preventing the regrowth of the cancer and improving survival time," says Alessandro Olivi, M.D., director of the Division of Neurosurgical Oncology at Hopkins and a contributor to the study.
Olivi says clinical studies using BMP4 could begin within a year and, if successful, drug therapies could be available to the public within three to four years.
"This was proof of the idea that BMPs could stop glioblastoma by depleting the stem-cell-like population that feeds it," says Henry Brem, M.D., chairman of the Department of Neurosurgery at Hopkins and a collaborator in the study. "This opens exciting doors to future research into treatments and therapies for such a devastating disease."
Source: Johns Hopkins Medical Institutions