Growth of spinal nerves is improved

Nerves that control the highest level of voluntary movements have been isolated and secrets of their growth revealed for the first time.
During development, these nerves extend themselves from the brain to all levels of the spine with the help of a potent growth factor called IGF-1. This factor is well known to scientists. However, the discovery of its role in guiding the extension of the longest nerves in the body was a big surprise.
The discovery has researchers talking about new ways to treat ALS, or Lou Gehrig's disease, and other paralyzing disorders, as well as regenerating spinal nerves that have been damaged by falls, crashes, and combat.
"Our experiments are highly relevant to understanding the basic development of the central nervous system of humans and other mammals," says Jeffrey Macklis, director of the Massachusetts General Hospital-Harvard Medical School Center for Nervous System Repair. "Learning how these nerves, known as corticospinal motor neurons (CSMN), establish connections between the brain and spinal cord could help find new treatments for ALS and other diseases caused by nerve degeneration. Such knowledge might also contribute to efforts to repair spinal-cord injuries." These goals, still many years away, might be accomplished by regrowing damaged nerves or recruiting new nerves from adult stem cells.
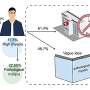
Macklis and postdoctoral fellow Hande Ozdinler isolated the long motor neurons from a tangle of look-alike nerve cells in the brains of mice. They kept the cells alive in laboratory dishes then bathed them in IGF-1. They also put tiny beads carrying the growth factor next to the nerves and made microscopic movies of what happened. "The results were immediate," Macklis recalls. "Within 30 seconds, we saw a dramatic outgrowth of the axons [nerve extensions]. IFG-1 increased their rate of growth a striking 15 to 20 fold."
Since these kinds of experiments cannot be done on humans, mice were used. "Mice mimic many aspects of human biology on molecular and genetic levels," Macklis points out. He sees the cells that survive but do not grow in lab dishes as mimicking motor neurons in adults. Reintroducing them to IGF-1 is like turning the biological clock back to infancy, when brain development is at its swiftest, and a baby is moving from uncoordinated flailing to drawing with crayons.
Reaching out
These experiments are part of an ongoing effort by Macklis and many others to determine how specific types of neurons form from unspecialized precursor or stem cells during the development of the human brain. "We want to dissect the brain one cell type at a time to uncover the many gears and cranks that make it work," he says.
The bodies of CSMN cells sit in the cerebral cortex, the largest most developed part of the brain. From there they send out long hairlike extensions called axons. In a fully formed human, an axon reaching down to the lower spine is as long as three feet. The brain uses these connections to communicate with the nerves that move fingers and legs in tasks like writing, sketching, and playing sports. When such connections are cut off in ALS and other diseases or because of injuries, the brain cannot make the body do what it wants to do.
Using techniques devised in their laboratory, Ozdinler and Macklis labeled target neurons from the spinal cord with fluorescent markers, then worked backward to the brain to sort and separate them into collections of pure CSMN cells that could be nurtured in laboratory dishes. They describe these efforts in the November issue of Nature Neuroscience.
Speeding up the messages
Once they uncovered the gears and cranks involved in tweaking CSMN growth, the researchers carefully disabled each one in mice. Things happened or didn't happen in the animals the same way as in the dishes. When IGF-1 was added to other types of nerves, no sudden or startling increase in axon growth was found. "This convinced us that we were seeing the 'real biology' of how these neurons connect the brain to the spinal cord," Macklis notes.
During development, CSMN axons reach out at the rate of about a half-inch in 10 days. After a week or two, the rate slows precipitously to approximately one inch in 25 weeks. In a developing baby, these nerves extend themselves from the brain to the spine in just a few weeks.
At the much slower rate of growth and with the longer distance to cover in adults, such extensions might require several years. "A neuron will not survive that long if its axon hasn't reached its target in the spinal cord," Macklis points out. "With the IGF-1 potential to increase growth rates 10 to 20 fold, one could imagine future treatments that may cut that time to months."
At this point, researchers can only imagine such a shortcut. There's too much to learn before it becomes a reality. For instance, what are the "seeing-eye" molecules that guide a nerve extension from the brain to the spinal cord? Some molecules that direct axon traffic are already known. They can attract or repel nerve endings or steer them left or right. However, the specific CSMN guides remain a mystery. "We are actively involved in looking for them," Macklis says with a note of urgency.
Once that kind of information becomes known, what happens in laboratory mice might be induced to happen in disabled humans.
Macklis, who is also head of the Nervous System Disease Program of the Harvard Stem Cell Institute, looks to recruiting new neurons from adult stem cells, present in small numbers in all adults. Using the right control molecules and growth factors, such cells might be coaxed into developing into new motor neurons that grow from the brain to the spinal cord. Another way to do this might be to take adult stem cells out of a patient, give the cells the character and growing ability they need, then transplant them back into the brain.
Macklis, Ozdinler, and others believe that such goals can be reached in the future. Progress made so far convinces them the damage that takes away the ability of people to move the way they want to move can be repaired.
Source: Harvard University