Mobile software to improve health care accessibility
According to the United Nations Foundation, there are about 5 billion mobile-device subscribers worldwide. Two-thirds of those are in low- and middle-income countries, many of whose citizens lack easy access to health care and must travel great distances — often hundreds of miles — to the nearest medical clinic.
Now, a team of student and faculty volunteers based at MIT’s Computer Science and Artificial Intelligence Laboratory (CSAIL) under the guidance of Peter Szolovits, professor of computer science and engineering and of health science and technology, has developed a way to use mobile-device technology to improve health-care access in developing countries. Known as Sana, which means “healthy” in Spanish and Italian, the open-source software system relies on smart phones running Google’s Android operating system to connect health-care workers in rural regions with physicians in urban areas. Using the Sana application on their phones, the workers collect patient data, including pictures and video, and send them in a text message to an electronic -record database. A doctor then reviews the data and sends a preliminary diagnosis to the health-care worker by text.
The Sana system, which includes at least one smart phone and a Web-connected server, grew out of an MIT NextLab class and another mobile-technology class taught by Hal Abelson, the Class of 1922 Professor of Computer Science and Engineering, offered in 2008. Several students from both classes developed the software code for Sana and formed a volunteer organization to distribute the code for free and help deploy Sana in developing countries.
Team member Crystal Mao ’10 discussed the system last week during a roundtable discussion held as part of the United Nations Summit on the Millennium Development Goals. She said Sana is part of a growing effort known as “telemedicine” that enables physicians to provide health care to patients through electronic or digital means. Doctors participate either because they are salaried employees of a country’s public-health system, and telemedicine is part of their responsibilities, or because they work for a company that provides telemedicine and uses a fee-for-service model. The doctor fee is included in the charges to the patients. Some physicians in urban areas donate their time out of personal interest in helping patients in rural areas.
‘A shared responsibility’
Sana (formerly known as Moca) joins a slew of mobile-health solutions that are targeted at the developing world, including ChildCount+, an application aimed at improving child survival and maternal health by using text messages to coordinate community health-care workers who use phones to register patients and report their health status to central web dashboard.
Like Sana, several of these emerging mobile-health efforts began at MIT; among them is Click Diagnostics, which is focused on the effective implementation of mobile-health software rather than the software design. What differentiates Sana from these other systems is its capacity to collect and transmit complex medical data including X-rays, ultrasound images, photos and electrocardiograms (ECGs), and then archiving this information into an electronic medical system.
This summer, several members of the Sana team, which includes about 20 undergraduate and graduate students and faculty from MIT, Harvard and other institutions, traveled to India and the Philippines to train health-care workers and developers on how to use Sana and to stimulate interest among the local developer communities.
This on-the-ground training and outreach to government officials, public-health schools, the telecommunications industry and software-development stakeholders is essential to Sana’s long-term success, says Leo Anthony Celi, a research scientist at the Harvard-MIT Division of Health Sciences and Technology (HST) who co-founded Sana. “[Sana] is really about training other countries rather than just giving them the technology,” Celi says, explaining that technology alone cannot overhaul health-care delivery.
Getachew Sahlu, a program manager for the World Health Organization, believes this mindset is what sets Sana apart from other mobile-health efforts. “What makes Sana unique is that the solution development and implementation is a shared responsibility with local stakeholders, which ensures sustainability,” he says.
During July and August, John Blakeney, a senior majoring in mathematics, and Chris Moses, who graduated from MIT in June, traveled to the Philippines to train developers to write software code for the system. This training is important because Sana is designed so that local developers can customize it to suit a region’s needs. The pair also traveled to a remote village to train health-care workers to use Sana. After helping the workers collect data from about 40 patients, Blakeney and Moses assisted with providing medications for the patients and asked for feedback about Sana.
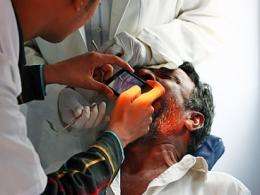
RJ Ryan, a CSAIL graduate student, traveled to India this summer to help several hospitals set up early cancer detection program. As part of his work, he and another Sana member, Harvard Business School student Sidhant Jena, helped create a way for health-care workers in Bangalore to use Sana to screen patients for oral cancer. The project involved taking photos of the mouths of 400 high-risk patients who were selected from 4,000 people identified during an initial screening, and using the application to send those images to an oncologist at the Narayana Hrudayalaya Hospital to look for lesions. As a result, the workers successfully referred two patients for treatment of precancerous lesions; it was Sana’s first direct success.
Improving Sana
The summer trips also identified areas for improvement, including the need for data-encryption capabilities for security purposes, as well as the ability to reconfigure phones remotely. In terms of operations, the Sana team needs to assign more defined roles and responsibilities for members and to figure out how to ensure sustainability as its members graduate, says Moses.
Sahlu sees another drawback to Sana: the relatively high cost of devices that run Android. Celi estimates that an Android phone would cost between $365 and $725 in the Philippines and between $120 and $250 in India (regular mobile phones start at about $30 in the Philippines and $20 in India, in comparison). Sahlu believes this will be Sana’s biggest challenge as more mobile-health solutions emerge that claim to offer the same or more functionality at a lower cost.
That issue is likely to be addressed in a new class about mobile health that will be offered next spring. Taught by mobile-health experts assembled by the Sana team, the course will focus on best practices in the implementation and evaluation of mobile-health technology from a public -health perspective. “It’s really about setting the standards now since there’s nothing currently in place in the developing world,” Celi explains.
In January, the next batch of Sana team members will continue to establish partners and hopefully scale the applications in India and the Philippines.
This story is republished courtesy of MIT News (web.mit.edu/newsoffice/), a popular site that covers news about MIT research, innovation and teaching.















