Do unruptured brain vessel malformations need preventative surgery?
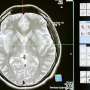
Individuals diagnosed with a brain arteriovenous malformation (AVM), an abnormal tangle of arteries and veins, are at an increased risk of vessel rupture and bleeding that can cause stroke and permanent brain damage.
Traditionally, doctors have advocated preventative interventions, such as endovascular procedures, surgical resection, or radiation therapy, and sometimes a combination of these procedures, on the assumption that unruptured AVMs pose similar risk to AVMs that have bled. By removing the unruptured AVM, this will decrease the risk of hemorrhaging and provide patient's better outcomes.
However, more recent data suggests that the risk of brain hemorrhage from unruptured or accidentally discovered brain AVMs may actually be lower and less severe than initially believed.
Now, Rush University Medical Center is part of an international, multicenter, NIH-funded trial called, "A Randomized Unruptured Brain Arteriovenous Malformation (ARUBA)," which is the first randomized, clinical study to evaluate whether a hands-off approach or intervention using any combination of endovascular, neurosurgical, or radiation therapy is better for managing an AVM that has not ruptured.
"The risk of having an AVM is that it could potentially rupture, bleed, injure the brain, and cause symptoms of stroke," said Dr. Michael Chen, neuroendovascular surgeon at Rush University Medical Center, and site principal investigator of the study. "However, removing or closing up a brain AVM by means of surgery, radiation therapy or interventional therapy may also potentially injure brain tissue and cause a stroke."
"Learning that you have an AVM can be a traumatic experience for patients. They may fear they are walking around with a ticking time bomb in their head," said Chen, who also is an assistant professor in neurology, neurosurgery and radiology at Rush University. "But we do not really know how likely it is that an unruptured AVM will bleed or if it ever will."
Past research has suggested that the annual risk of hemorrhaging in the brain from unruptured AVMs may be as low as one percent per year especially among those for whom intervention appears feasible. But large and more complex AVMs have higher hemorrhage rates and pose greater technical challenges for intervention, and as a result treatment is deferred for many due to the risks. Age, deep brain location, associated aneurysms, and deep venous drainage add to hemorrhage risk factors.
"We hope that this study will provide high-quality, scientific evidence to guide the often times difficult decision on whether one ought to have preventative treatment," said Chen. "Currently, this decision is largely determined by anecdotal experiences, biases, hopes and fears."
Patients enrolled in the study will be randomly assigned to one of two groups - those who will undergo an AVM elimination and those who will only be managed medically. Study participants will be followed for 5-8 years.
The ARUBA study has enrolled over 120 patients and plants to enroll 800 patients from 100 different institutions worldwide. Rush is one of only two Chicago area medical centers participating in the study.
About Brain Arteriovenous Malformations
Arteriovenous malformations of the brain (AVMs) are abnormal tangles of arteries and veins which usually date back to birth, but can also result from head injury. Brain AVMs can occur in any part of the brain and what causes them is not clear.
Normally, blood from the heart moves from the arteries to the veins through a fine network of small blood vessels called a capillary bed. In an individual with a brain AVM, the arteries and veins are connected directly without a capillary bed, exposing the thin-walled veins to high pressure that increase risk for rupturing and bleeding into the brain.
You may not know you have an AVM until you experience symptoms, such as headaches or a seizure. In serious cases, the blood vessels rupture, causing bleeding in the brain (hemorrhage).
A brain AVM often causes no signs or symptoms until the AVM ruptures, resulting in bleeding in the brain (hemorrhage). A bleeding AVM in the brain is life-threatening and requires emergency medical attention.