Vanderbilt Lung Cancer Trial for Never Smokers Goes Online

(PhysOrg.com) -- One of the enduring mysteries of lung cancer is why so many people who never smoked develop the disease. More than 219,000 patients are diagnosed with lung cancer in the United States every year, according to the National Cancer Institute. About 20,000 - one in 10 - never smoked tobacco products. Most of those patients are women.
One of the enduring mysteries of lung cancer is why so many people who never smoked develop the disease. More than 219,000 patients are diagnosed with lung cancer in the United States every year, according to the National Cancer Institute. About 20,000 - one in 10 - never smoked tobacco products. Most of those patients are women.
Since tobacco exposure is the strongest known risk factor for lung cancer, researchers believe genetic differences may make some of these “never smokers” more likely to develop the disease.
William Pao, M.D., Ph.D., assistant director of Personalized Cancer Medicine at Vanderbilt-Ingram Cancer Center, is inviting those never smoker patients already with lung cancer to join a Web-based clinical trial to search for those genetic differences.
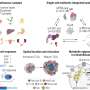
“Our goal is to look at the DNA in blood or saliva samples as part of a future genome-wide association study,” said Pao, Ingram Associate Professor of Cancer Research. “You can look at more than half a million areas in the DNA where people may differ. When we start to see patterns in the DNA of patients like never smokers, we can take a closer look and try to identify genetic mutations that may be important in the lung cancer disease process.”
Pao and his colleagues hope to collect 2,000 DNA specimens from never smokers with lung cancer, who are defined as having lung cancer and smoking fewer than 100 cigarettes in their lifetime. Since a single cancer center doesn’t see enough never smoker lung cancer patients in a year to collect a large number of specimens, Pao turned to the Web to recruit patients.
“We believe this is the first study in a solid tumor cancer to try to collect blood specimens through an online process,” said Pao. “Patients can go to our Web site, fill out a simple electronic questionnaire, and if they qualify for the clinical trial we will ship them two empty blood vials. The next time they visit their doctor for a blood draw, they can get those vials filled and ship them to us via UPS and we will pay the shipping costs. For those patients who can’t get the blood drawn, there is also an option of using saliva samples.”
To protect patient privacy, the DNA samples are de-identified when they are entered into the Vanderbilt-Ingram DNA databank, a secured databank designed to prevent tracing samples back to a specific donor.
“It is possible that there is some genetic susceptibility among never smokers with lung cancer that makes them more likely to develop the disease,” explained Pao. “They are not necessarily born with a predetermination that they will get lung cancer, but they may be born with certain genes that predispose them if they are exposed to some environmental toxins.”
Pao and other lung cancer investigators feel a sense of urgency because they still don’t know enough about the genetic pathways that are important in the development and spread of the disease. According to the American Cancer Society, fewer than 20 percent of lung cancer patients are still alive five years after diagnosis.
“More than half of all lung cancer patients are diagnosed in the incurable stage, so we’re already on the losing side of the battle with too many patients by the time we detect the cancer,” explained Pao.
“Eventually, this kind of study may help us identify genetic targets that allow us to develop simple blood tests to detect cancer early. Those same targets could be used to develop drugs that block or interfere with the disease process.”
For more information, visit www.vicc.org/neversmokers
Provided by Vanderbilt Medical Center