Brain Defect Implicated in Early Schizophrenia
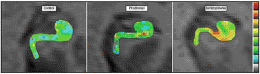
(PhysOrg.com) -- In the first functional magnetic resonance imaging (fMRI) study of its kind, neurologists and psychiatrists at Columbia University have identified an area of the brain involved in the earliest stages of schizophrenia and related psychotic disorders.
Activity in this specific region of the hippocampus may help predict the onset of the disease, offering opportunities for earlier diagnosis and for the development of drugs for schizophrenia prevention.
Details of the findings were published in the September 7, 2009, issue of Archives of General Psychiatry.
In the study, the researchers scanned the brains of 18 high-risk individuals with "prodromal"
symptoms, and followed them for two years. Of those individuals who went on to develop first-episode psychotic disorders such as schizophrenia, 70 percent had unusually high activity in this region of the hippocampus, known as the CA1 subfield.
While previous studies have identified a more general increase in activity in the hippocampus in chronic schizophrenia, this study shows that in the early stages of the illness, before symptoms are fully manifest, this increased activity is evident only in this one subregion and can distinguish who among high-risk individuals will go on to develop these disorders.
Functional magnetic resonance imaging is a non-invasive technique that measures brain metabolism,
indicating what parts of the brain are active during which activities. Mapping cerebral blood
volume (CBV) is a method used in fMRI to measure this activity and it indicates increases or decreases in metabolism.
Using a novel high-resolution application of fMRI, pioneered by lead study investigator Scott A. Small, M.D., the researchers first compared 18 patients with schizophrenia to 18 healthy controls and observed abnormalities in multiple areas of the brains of the patients with schizophrenia.
Next, to learn which of those regions of the brain were targeted first in patients with first-episode psychotic
disorders, like schizophrenia, the investigators imaged young people identified as at high risk for psychosis, who were then followed for two years to determine diagnostic outcome.
"By applying this imaging technology to a population of high-risk individuals, we wanted to see if we could find an area of the brain that is selectively targeted," said first author Scott A. Schobel, M.D., assistant professor of clinical psychiatry at Columbia and the New York State Psychiatric Institute. "In comparing those high-risk individuals who developed psychosis with those who did not, we found that only the CA1 subfield was abnormal in those young people who went on to develop schizophrenia. We believe that this may give us an early snapshot of disease."
"What many brain disorders have in common is that they are all relatively invisible to conventional imaging techniques," said Dr. Small, Herbert Irving Associate Professor of Neurology in the Sergievsky Center and in the Taub Institute for Research on Alzheimer's Disease and the Aging Brain at Columbia University Medical Center. "It is crucial to be able to visualize the most affected area of the brain and to pinpoint the region that is most vulnerable. This will give us clues into the causes of the disease.
"Our findings could help us improve diagnosis in the preclinical stage, which is most important because it is this stage of the disease that will be most amenable to treatment," said Dr. Small.
Currently, no tests are available to diagnose schizophrenia. Diagnosis is mostly based on clinical symptoms after tests to rule out other possible causes. "Right now, the odds of knowing who will go on to develop
schizophrenia from the prodromal stage is only a little better than a coin toss," said Dr. Schobel.
To meet the criteria for a prodromal group, subjects need to present with what clinicians call "subthreshold"
psychotic symptoms. "These involve illusions (hearing one's name in the wind) rather than hallucinations (hearing voices) or overvalued unusual ideas that lack the conviction of clear delusions, such as feeling suspicious of others but without a sense of being singled out or persecuted," said Cheryl Corcoran, M.D., Irving Assistant Professor of Clinical Psychiatry and director of the Center for Prevention and Evaluation, a prodromal research program at Columbia and the New York State Psychiatric Institute.
"Persons who have a family member with a known psychotic disorder, and also experience some kind of social
withdrawal, would also meet the criteria, as would an individual who shows up at the emergency room with a temporary full-blown psychosis," said Dr. Corcoran.
Of a typical prodromal cohort, approximately 35 percent will go on to develop a full-blown psychotic disorder, usually schizophrenia, at 2.5 years. "We're hoping that applying this imaging technique can enhance our knowledge of who might go on to develop schizophrenia and related disorders, since early diagnosis and early intervention are so important," said Dr. Schobel.
"We're now trying to understand why CA1 is selectively targeted. We need to ask what is the underlying cause and to find a pattern and investigate why this area is affected first. It may be that the CA1 subfield is also driving dysfunction in other brain regions in establishing the illness," said Dr. Small.
Despite the strength of the findings in this small population of patients, imaging of a larger group and replication of the findings are necessary to clarify how accurate and specific this is for diagnosing preclinical schizophrenia.
"A larger study will determine if this is really a true biomarker that can be used as a diagnostic tool for identifying risk for schizophrenia on an individual basis," said Dr. Small.
Contrary to popular belief, schizophrenia is not a split personality; it is a chronic, severe, and disabling brain disorder that affects just over 1 percent of the adult population and is characterized by loss of contact with reality (psychosis), hallucinations (usually, hearing voices), firmly held false beliefs (delusions), abnormal thinking, a restricted range of emotions (flattened affect) or inappropriate and disorganized behavior, social withdrawal, and diminished motivation.
The disease often strikes in the early adult years, and although many individuals experience some recovery, many others experience substantial and lifelong disability. People with schizophrenia often have problems functioning in society and in relationships and are over-represented on disability rolls and among the homeless and imprisoned.
What precisely causes schizophrenia is not known, but current research suggests a combination of hereditary and environmental factors. Fundamentally, however, it is a biologic problem (involving changes in the brain), not one caused by poor parenting or a mentally unhealthy environment.
"Research has shown that early intervention and treatment can prevent the debilitating effects of schizophrenia by dramatically slowing progression, reducing mortality and disability, and increasing recovery of one of mankind's most costly mental disorders," said Jeffrey A. Lieberman, M.D., a renowned expert in the field of schizophrenia, who has recently been selected by the National
Institute of Mental Health (NIMH) of the National Institutes of Health to lead a nationwide effort to develop an optimal early intervention strategy for treating people experiencing a first-episode of the psychotic symptoms of schizophrenia.
Source: Columbia University Medical Center (news : web)















